See the Bigger Picture
Information sharing between eyecare professionals is far more difficult than it should be. How do we improve it?
Dawn Sim |
At a Glance
- It’s remarkable, that still today, patients resort to taking photos of OCT images and retina scans acquired by their optometrist to share with their ophthalmologist
- This is due to a lack of integrated systems that allow referrers to easily communicate with ophthalmologists
- What’s needed is a system that’s image platform-agnostic; a cloud-based solution that accepts multiple, standardized formats
- Such a system is about to be tested in the UK and the hope is that software like this will enhance collaborative care, improve the patient pathway and pave the way for new technologies
It’s an exciting time to be working in ophthalmology. Advances in imaging technology are revealing more about ocular disease, and the combination of “big data” and artificial intelligence strategies (such as Moorfields and Google DeepMind Health’s recent collaboration) is set to transform the diagnosis and detection of disease from images of the eye. However, a crucial ingredient for the successful integration of these technical advances into the real world of clinical practice is the existence of platforms that accommodate them, and the foresight of building infrastructure to support these promising technologies. A natural starting point for this, I believe, will be in the field of teleophthalmology, which relies heavily on both acquiring images of the eye and an electronic means to review, report, and relay information to the patient. In an ideal setting, an image will be acquired in a place convenient to the patient and an artificial intelligence algorithm will read the scans and generate an instantaneous report for the patient. A remotely located expert in the relevant ophthalmic subspecialty could then validate this report, communicate health advice to the patient and/or advise the need for a face-to-face encounter or repeat scan. Arguably, this utopia is within our reach today, but understanding its barriers and identifying practical solutions will be key in realizing this in our day-to-day practice.
Learning lessons from radiology
In a typical workflow, a patient will see an optometrist or a general practitioner (GP) – or both – before being referred to an ophthalmologist. But as they move along their patient journey, it seems that no-one is sharing their eye images. Incompatible file formats and image management systems along that patient journey can mean that there is no easy way for ophthalmologists to quickly access high-quality image scans. Occasionally, referrals may come to an ophthalmologist with a poor quality image – often, as a black and white grainy printout, or a single snapshot of an OCT scan (as opposed to the 100 image volume scan of the macula), or worse, a smartphone photo of a scan acquired by the patient or a relative. These archaic methods of communication is not only insufficient for effective triage, it renders the pursuit of collaborative care or new technology adoption invalid. It also creates more work – if there’s any ambiguity at all, you absolutely need to perform your own OCT scans and retinal photographs.
One of the main barriers holding us back is legacy technology. Something as simple as an OCT image cannot be read using the proprietary platforms provided by the different OCT manufacturers – and in many cases, the imaging data is encrypted! This is reminiscent of the situation that radiology was in more than 30 years ago; where radiologists using different imaging devices could not decode or share their images. However, the disruptive technology of computerized tomography (CT) and magnetic resonance imaging (MRI) scans that all but made single frame X-rays obsolete, proved a tipping point for the field. This era saw the development of Digital Imaging and Communications in Medicine (DICOM) – a means of standardizing medical imaging and patient information across different devices. DICOM was first co-developed in 1985 by the American College of Radiology and the National Electrical Manufacturers Association, yet it took almost 10 years to take its current form today; an almost universally accepted industry communications standard for medical images. DICOM (as with any industry standard) has its limitations, however it has created an interoperable and open system that has been central to advancements in the field of radiology.
Ophthalmologists now face a similar challenge but in a very different time. We are at the height of the digital age, as compared with our radiology colleagues who broached this problem when the World Wide Web was merely a toddler. Surely we can make our OCTs, visual fields, and autorefractometers talk to each other and feed into an electronic health record system? It is therefore incongruous that this hard-won interoperability seems a lot easier in radiology than in ophthalmology. In reality, an ophthalmic DICOM does exist, but it is used by few, and many OCT manufacturers continue to utilize closed formats that require users to “pay extra” for DICOM capabilities. As tech-loving ophthalmologists, we are naturally lured by new inventions – the promise of a higher definition scan, improved motion tracking, instantaneous 3D rendering. In effect, for these big tech dreams to be realized we must concurrently build infrastructure and platforms to bring this to our patients.
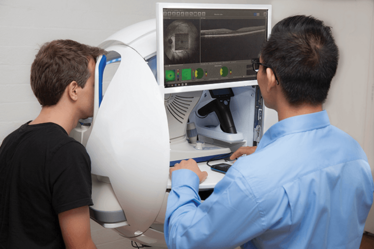

Example of an Automated Patient Journey
Step One
Customer visits primary healthcare provider who scans their eye at a kiosk, which incorporates advanced eye scanning technology including OCT. Scans are then instantly and securely uploaded to the cloud-based platform.
Step Two
Customer eye scans and relevant history are reviewed and reported on remotely by eyecare specialists.
Step Three
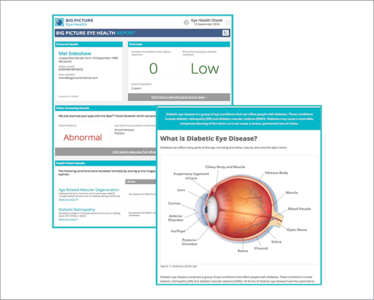
Using input from specialists, the software automatically generates a detailed eye health report for the patient, including educational content and a referral to an ophthalmologist, or optometrist if necessary. The detailed report can be shared with any healthcare provider participating in the patients care.
Could we have a solution?
I was introduced to a software company based in Sydney that had the foresight to develop such a platform to solve this problem. Big Picture Eye Health was founded by Tom McKinnon, a medical practitioner who saw the crevice between new technology and integrative platforms, and he hopes to revolutionize how images are taken, assessed, and reported on by eyecare specialists.
The primary aim of Big Picture was to find a solution for streamlining the patient’s eyecare journey – to develop a platform that covers the entire pathway and works with all imaging devices. Over the past three years, his team of software engineers and physicians have been working on developing exactly this – an interoperable software platform, integrating eyecare expertise with advanced eye scanning technology and decision support algorithms. The platform combines multiple elements of comprehensive eyecare; an iPad-based patient registration, patient-directed consent and history taking, remotely controlled eye scanning equipment, image compression technology and software diagnostics culminating in a cloud platform for scan review, referral management and patient communication. Although the platform is capable of performing eye scans, one of its most important features is that it is fully DICOM compliant and works with all medical imaging devices.
The platform stores all patient scans and information in a single secure location and can be accessed from anywhere through a web browser. This not only facilitates international collaboration, but also should be invaluable for the increased global mobility of patients, as it offers patients ownership and freedom of control of their own eye scans and health data, while ensuring that no information is lost along their eyecare pathway. As research has shown that many patients leave medical consults not really knowing what the plan is or where to go from there, the platform’s personalized online portal would mean that patients will not only be able to access their actual eye scans, but also review a summary of their care, details of the follow up plan, and relevant educational materials. (See Sidebar: Example of an Automated Patient Journey). Another element of the software is its structured approach to analysis and reporting, which includes a user-friendly interface for referral, according to patient location and support algorithms that calculate validated risk scores – these risk scores are based on parameters such as age, duration of diabetes, HbA1c etc., and are available to both patients and eye specialists. In the future, the platform may also be used as a personalized health education tool.
Ophthalmology in the cloud
Empowered patients are increasingly demanding convenience – healthcare services need to be accessible, efficient and of a high quality. To avoid lengthy waits in the eye clinic, a model of eyecare that incorporates teleophthalmology into routine clinical practice means that patients could be monitored more frequently than they are now. For example, a patient with high risk dry age-related macula degeneration (AMD) could choose to have an OCT scan every month, then have that scan reviewed and the results reported back to them by their own ophthalmologist. The patient would only need to see their specialist once or twice a year, and yet have their eyes closely monitored; this would allow conversion to wet AMD to be detected early, and facilitate rapid commencement of therapy. For those without known eye disease, this form of opportunistic screening may uncover refractive errors or eye pathology that would benefit from visual aids and/or specialist intervention.
Looking ahead
The platform is scheduled to launch in Australia before the end of the year, and will be accompanied by an all-in-one eye imaging kiosk, which includes OCT, fundus cameras, autorefractors, and visual field assessments. With their kiosk situated in the community and the cloud-based platform, Big Picture will be the first in the world to attempt to make one interoperable platform that seamlessly covers the entire patient journey. A collaborative study between the company and Moorfields Eye Hospital is also planned to take place in the United Kingdom, and let’s hope that this software is the first of many new technologies that our industry will embrace to drive significant improvement in the way that critical eyecare information is accessed and communicated amongst professionals – all in the name of better patient care.
Dawn Sim is a Consultant Ophthalmologist at Moorfields Eye Hospital, and Institute of Ophthalmology, University College London, United Kingdom, and Global Medical Lead of Big Picture Eye Health.
Dawn Sim is a Consultant Ophthalmologist at Moorfields Eye Hospital, and Institute of Ophthalmology, University College London, United Kingdom, and Global Medical Lead of Big Picture Eye Health.













