
- FLACS is as safe and effective as manual cataract surgery – but some practices struggle with its integration, with uptake relying on effective internal and external marketing, well-structured refractive packages and optimized practice workflow
- Successful conversions often start long before the patient even walks through the door, by planting the seed with primary eye care doctors who are referring patients for surgery
- Once the patient is on-board, surgeons should stress the undeniable benefits of FLACS: precision, reproducibility and automation
- Don’t be afraid to talk costs at the initial consult – it puts the patients at ease and gives them the information they need to make a measured decision, saving you and your refractive counselor’s time.
Approximately 65 percent of patients undergoing cataract surgery in our practice choose to have femtosecond laser-assisted cataract surgery (FLACS) – a relatively high conversion rate, given the low mean household income in the market in which I practice. It’s not a new thing either. We’ve been consistently reaching this high conversion rate since we launched FLACS, and we’ve done it without any level of effort I’d consider extraordinary.
On the contrary, it was a very natural and organic fit for our practice and the mindset of our team. So how is this possible? I believe it’s due to a number of factors, including effective internal and external marketing, the way we structure refractive packages and our workflow. However, by far the most important factor is how my partners and I personally view the value of the laser. Put simply, we believe this technology helps us better serve patients. If we didn’t, we wouldn’t offer it.
It’s not that manual is bad; I actually think manual surgery is fantastic! I know that I can perform an excellent manual cataract surgery and I have colleagues who I would trust to perform excellent manual surgery, as well. But I also know that I chose the laser for my own mother and that’s what I would want if I were having cataract surgery. This simple, non-emotional, non-political fact forms the foundation of how I talk about FLACS to patients.
We don’t give patients a “hard sell” and we don’t tell them the laser is safer or that they will necessarily see better by choosing the laser. We don’t need to do that. Instead, we simply talk about the laser’s precision, reproducibility, and automation. As a surgeon, I believe that precision matters, so an honest conversation about femtosecond laser technology follows easily from that belief.
I believe too many surgeons get caught up focusing on what technology doesn’t do instead of focusing on what it does do. I imagine many surgeons were soured by their experience with first-generation lasers, just like they were with first-generation presbyopia-correcting IOLs. But a decade has passed and lasers are better now.
I personally believe FLACS is safer and better than manual surgery – and newer research backs it up. Plenty of studies with modern lasers and newer software versions have shown safety data that FLACS is superior to manual (1); however, I understand there are also large meta-analysis studies that have found them to be equivalent. I believe this will follow a similar trajectory as the evolution of extracapsular surgery to phacoemulsification.
In the beginning, even when the data wasn’t overwhelmingly in support of phaco, early pioneers pushed on because they intuitively knew it was better. They saw it every day in their own ORs. They just felt it. The patient’s visual goals are also an important part of the conversation, because FLACS is automatically included in each of our refractive, advanced-technology packages.
I like to keep it simple by offering patients just three packages. Keeping it simple helps our patients avoid “paralysis by analysis,” where too many options make it too difficult to come to a decision. Our three options for cataract surgery include:
- Option 1: Manual cataract surgery with a monofocal lens and no astigmatism correction. Patients should expect to need bifocal glasses after surgery. I always make a point to mention that it is good and safe surgery, even if the patient starts out the consult by expressing interest in FLACS and advanced IOLs. I do this because I sleep comfortably at night knowing that no patient can ever say that I “talked them into” upgrading to FLACS.
- Option 2: FLACS with astigmatism correction, whether that be with astigmatic keratotomy or a toric lens. This option also includes ORA intraoperative aberrometry (Alcon). We tell patients that with this option they will likely be able to see at distance without wearing spectacles or contact lenses, but will need reading glasses for their up-close vision.
- Option 3: FLACS with correction for astigmatism and a presbyopia-correcting IOL. We tell patients this will greatly reduce their need for glasses at all distances. Option 3 includes ORA, as well as a LASIK touch-up within the first year if needed. Patients like knowing they have that safety net; it increases their confidence in reaching their refractive goals.
Some practices have struggled with FLACS conversion because they present patients with the option just once, discuss it too late in the decision process, fail to provide enough context or fail to make a recommendation. We believe in including discussions of laser cataract surgery early and often – ensuring there are no surprises.
Successful conversions start long before the patient even walks through the door, by planting the seed with primary eye care doctors who are referring patients for surgery. The seven optometrists who work for Williamson Eye and our referring optometrists outside the practice all know my views on the value of the femtosecond laser…and they share those views as I’ve used FLACS to operate on them personally or their loved ones in several instances. So it’s one of the things they will mention when they first diagnose a patient with cataract.
They have also told me they enjoy seeing these patients postoperatively because of the fast visual recovery and “wow” effect. When a patient schedules a cataract surgery consultation with us, they get an information packet that includes a pamphlet about the laser we use (Catalys, Johnson & Johnson Vision), as well as the available IOL options.
We are proud of our advanced technology options and don’t hesitate to promote them within the practice. For example, we have custom-made, seven-foot-tall banners next to every check-in station educating patients about the Catalys laser and other technologies that we use (Figure 1). Every single person who comes into Williamson Eye Center sees those banners, whether they are here for an eye exam, dry eye treatment or bringing in a relative for LASIK surgery. I also have posters in the exam lanes on either side of the eye chart featuring the laser and advanced IOL options.
Most importantly, we have created a video about FLACS to standardize the information patients receive about what the femtosecond laser is and how it helps us better meet their needs. We have many ophthalmologists, optometrists and staff members at our practice, so the video helps ensure that patients’ awareness of FLACS isn’t dependent on how passionate or articulate one person is compared with another.
The eight-minute video was filmed and produced by students from the local university so not only was it very economical, it was personalized to us, as opposed to the cartoon animation videos the laser company provides. Each of our surgeons has a speaking part (all of which were carefully scripted to convey the exact message we wanted) and the video features the procedure, an animation comparing the automation of the femtosecond laser with a manual cataract surgery and an overview of our three package options.
Patients watch the video on a large iPad after their workup (Figure 2), just before they see the surgeon. They also receive an oversized “menu” of the package options that reiterates what the video covers (Figure 3). When I walk in the room, I can feel confident that the patient is well educated about the different options, and I can tailor our conversation to my findings and answer their questions about surgery. Often, when I walk into a room the patient says “I’d like a number two!” The conversation is very streamlined from that point.


In talking about the package options, I like to use the analogy of buying a car or a new computer, because those are purchases many people would have made in the past few years. On a new car, you can choose from several trim packages. On a computer, you can get different software and features based on whether you plan to use it for gaming, for browsing or for work. I tell them that cataract surgery is similar in that there are options to customize vision based on your lifestyle and your visual goals.
All the options are safe and effective, but your choice centers on how much – or how little – you want to wear glasses. I also express the finality of this procedure by telling them it’s similar to a heart valve in that the implant will never come out. They can’t come back for an upgrade in five years, so it’s critical they choose the best technology for their visual goals.
Many surgeons dread discussing pricing and avoid it completely, preferring to let a patient counselor handle that part of the conversation. This works for some, but not others. Initially, I thought that would be my approach, but I quickly realized that avoiding the cost conversation wasn’t equipping my patients with the realities they needed to make the decision and it wasn’t setting up my counselor for success either.
Often, they would have a great discussion with me about presbyopia IOL solutions, only to get to my counselor and experience sticker shock when they found out the lenses they want are more than they can afford. They leave upset, my counselor feels like she’s failed and sometimes these patients even end up at other practices.
Given this experience, I changed my approach. The bottom line is most cataract surgery candidates already take for granted they’re going to see well, so they have two basic questions left on their mind: Will it hurt? And how much does it cost? That’s what they are wondering throughout the entire hour-and-a-half diagnostic work-up. So when they finally get to me, I’d rather just address the elephant in the room by answering both of those questions. This puts the patients at ease and gives them a baseline understanding of cost so they can make a decision about value.
Here’s how my consult usually goes:
- I ask about how they like to use their eyes and what their visual goals are
- I talk about what else is wrong with their eyes besides cataract, like dry eye, macular degeneration or diabetic retinopathy and how these diseases will still be there after surgery (which lowers expectations)
- If they have astigmatism, I tell them that’s one of the only things I “can fix” at the time of cataract surgery and that doing so will reduce their need for bifocals
- I explain what they’re a candidate for
- If it sounds like they’re interested in option 2 or option 3 (and it’s medically appropriate), I walk them through what those premium packages include and don’t include
- I touch on price, explaining that while I can’t give them an exact number because it depends on their insurance, the ballpark monthly price for those who finance the surgery is X and the ballpark total cost if they pay for everything up front is Y
- I like to relate that monthly payment number to something mundane in their life like a round of groceries or a cable bill. They are often paying more for their internet than we are asking them to pay for their vision, which really puts things into perspective
- I reinforce that many patients take advantage of the no-interest financing we provide that allows them to pay by the month (but of course, they always have the option to pay in full)
- I also let them know that even with option 2 and 3, the non-refractive portions of the surgery will still be covered by insurance and that often this makes up the majority of the total cost
With this approach, most patients are able to make a decision right away. As I walk out, I tell my teammate: “Hey, she’s interested in option 2. This is what we’re going to do.” The counselor will then get into a lot more details about insurance coverage and deductibles, payment plans, and so on. If patients aren’t ready to make a decision at that moment, we reassure them they can take all the time they need to discuss this with their family and research their options. Their biometry and history and physical is generally performed two weeks after the consult, which gives me time to clean up their ocular surface and gives them time to consider their options without feeling rushed.
Marketing FLACS doesn’t end with the patient’s decision about what type of surgery to have. It’s also important that surgeons continue to refine their laser settings and techniques to actually deliver the highest level of precision possible and meet expectations for visual outcomes. To me, the primary clinical advantage of FLACS is that it automates and standardizes many of the variables in manual cataract surgery, similar to femtosecond laser LASIK compared with old microkeratomes.
My father taught me early on that in refractive surgery, “automation” is a good word and “variables” is a bad word. For instance, the capsulotomy size can be set very precisely, after accounting for some stretch. I like to set mine at about 4.9 millimetres, so that I end up with a capsulotomy of about 5.1 millimetres, sufficient to consistently cover the edge of the optic for all 360 degrees around. This provides at least some level of standardization for the effective lens position (ELP) and also reduces the potential for lens tilt when implanting a toric IOL. My capsulotomies are perfect and free floating 99 percent of the time. No human being can do that in less than one second, 2,000 times in a row, year in and year out.
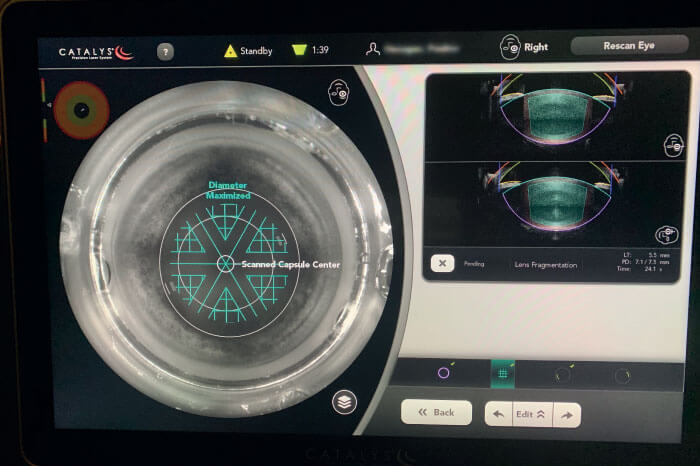
In addition to size, a well-centered capsulotomy is very important for ELP. I prefer to use the Catalys laser’s scanned capsule setting (Figure 4) to center the capsulotomy on the capsular bag where it will sit, rather than on the pupillary center. I often choose to make anterior penetrating astigmatic keratotomy (AK) incisions. Not only do I find these to be more effective and consistent than intrastromal non-penetrating incisions, but I also like having the ability to titrate the AKs intraoperatively, choosing to open them or not based on the intraoperative aberrometry measurements.
Although many surgeons will have preferred settings for routine cataracts, it is important to adjust settings for unusual cases. For instance, in a case with a denser nucleus, I increase the fragmentation to debulk the nucleus and reduce my phaco time. For white or black cataracts, as well as those with any corneal scarring, I increase the laser energy settings to ensure that I can penetrate through the corneal opacity and achieve a complete capsulotomy. The laser can’t treat what it can’t see, so achieving good fragmentation can be difficult in these cases, but having a perfect capsulotomy is always useful – especially when dealing with the densest cataracts.
Finally, it is absolutely essential to diagnose dry eye before surgery so patients know that the surgery didn’t cause it. Once you start really looking, you may be surprised to find that almost all cataract patients have dry eye, whether they present with complaints or not. Our workup includes point-of-care osmolarity and MMP-9 testing on all cataract evaluations, as well as tear break-up time with the HD Analyzer (Visiometrics) and a careful evaluation of the lids and meibomian glands.
We typically schedule patients within two to three weeks of their consult, so I immediately start almost all patients on preservative-free tears. For the vast majority of patients with inflammation and hyperosmolarity, I also prescribe an immunomodulator and loteprednol for a couple weeks before surgery.
Those with MGD may get thermal pulsation therapy or blepharoexfoliation. For patients with significant irregular astigmatism, I delay surgery to four weeks or more, so that we can repeat their topography and biometry after a longer course of dry eye therapy. Dry eye treatment alone can rule in or rule out advanced technology IOLs for these patients.
Done right, FLACS can be a lot of fun to integrate into your surgical processes and practice marketing. Together with advanced technology IOLs, the laser presents an opportunity to give patients the kind of visual outcomes and lifestyle benefits that many of us would choose for our own eyes. Let’s make sure our patients know that too.
References
- WJ Scott et al., “Comparison of vitreous loss rates between manual phacoemulsifcation and femtosecond laser assisted cataract surgery”, J Cataract Refract Surg, 42 (7), 1003-8 (2016). PMID: 27492098
