The idea of running an intensive phacoemulsification training program in Rwanda began with a simple email exchange. Olivia Earley reached out to ask if there was any way she could support the work in Rwanda. The conversation quickly turned to a practical question: could she come and help train two Rwandan ophthalmologists in phacoemulsification, who were recently graduated from the residency programme. They had established microsurgical skills, including manual small incision cataract surgery (MSICS).
Across much of sub-Saharan Africa, cataract surgery is still dominated by MSICS. It is safe, reliable, effective, and well suited to the realities of many healthcare systems. Phacoemulsification, on the other hand, is seen as difficult to introduce. It relies heavily on expensive technology, few training opportunities, complications carry a higher ocular morbidity, and subsequent interventional vitreoretinal surgical support is not always available.
Yet the demand to learn phaco is very real. Many African ophthalmologists want to develop these skills, not to replace MSICS, but to deliver more effective surgery to eyes more suited to phacoemulsification e.g. younger patients with immature cataracts.
Our recent study (1) described the experience of two ophthalmologists who undertook a four-week intensive phacoemulsification training program at Kabgayi Eye Unit in Rwanda. At the end of the four weeks, they performed 85 cases and had gained competency to perform full cases independently. However, this was not enough to deem them experienced, and this period was followed by twelve months of independent operating, supported by senior phaco surgeons. Over the following year they performed 754 cases with complication rates comparable to those reported internationally.

For us, however, the most important lesson was not simply that the training worked. It was why it worked.
Training works when the ecosystem is right
Kabgayi Eye Unit has several features that made this program possible: a high surgical volume, dedicated phaco machines, a wet-lab for simulation training, and experienced surgeons – including a vitreoretinal surgeon (VR) – operating side-by-side in an open-plan theatre. The proximity of senior surgeons working in the same space allowed them to step in quickly if help was needed, while still facilitating the trainees to gain independence and build surgical confidence. Together, these elements create an environment where skills can be developed quickly through repetition, supervision, and immediate feedback.
This kind of concentrated exposure may be particularly important in Africa, where the number of surgeons able to teach phacoemulsification is still relatively small. Intensive training allows visiting trainers to transfer foundational skills efficiently within a limited period of time.
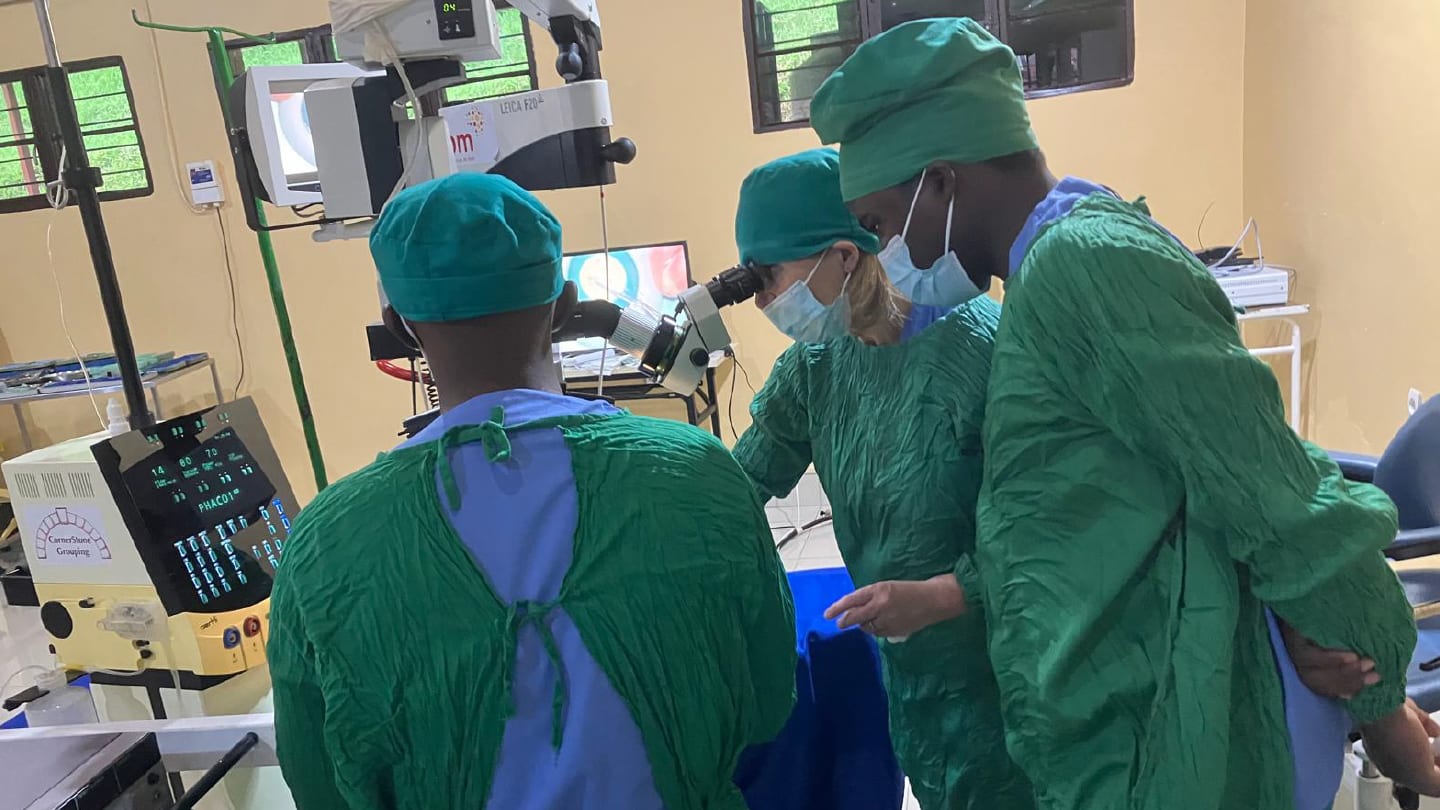
Four weeks does not create a phacoemulsification surgeon
In reality, the four-week program simply started the learning curve. During that time the trainees accumulated around 160 hours of deliberate practice. This was a small component of the recognized 10,000 hours requirement to truly master complex microsurgery (2).
The real progress happened during the 12 months that followed with building expertise in a safe supervised environment.
In many ways, this created a modern version of the traditional surgical apprenticeship – the intensive course provided the foundation, but sustained practice allowed the skills to become embedded.
The hidden pillar of phacoemulsification training
One particular lesson stood out very clearly during the program: the importance of VR support.
Complications such as posterior capsule rupture or dropped lens fragments are an inevitable part of the learning curve in phacoemulsification, and are recognized factors in delaying surgical progression. Introducing phaco without access to VR care risks leaving both trainees and patients vulnerable when complications occur. On the other hand, the presence of VR support creates a safety net that allows surgeons to learn with confidence. In parts of Africa, however, access to VR services still remains very limited.
During the training programme there were two complications that required vitreoretinal intervention: one dropped intraocular lens and one dropped nucleus. Because VR support was available on site, both patients were treated promptly and achieved good final visual outcomes.
Without that on-site support, the situation would have been very different, with the development of painful blind eyes for these patients.
This experience reinforced an important principle: phacoemulsification training and vitreoretinal services need to grow hand in hand. In this sense, the two services are not separate; they are parts of the same surgical ecosystem.
When trainees become trainers
One of the most encouraging developments that has evolved from this phacoemulsification training is that one of the trained surgeons has now taken the role of Trainer, as well as undertaking a VR fellowship. Sustainable surgical training does not depend on visiting experts alone. It depends on the growth of a local culture of teaching, where knowledge is passed on from one generation of surgeons to the next.
If that culture continues to grow, centres like Kabgayi may eventually serve as regional training hubs, supporting surgeons not only from Rwanda but also from neighboring countries.
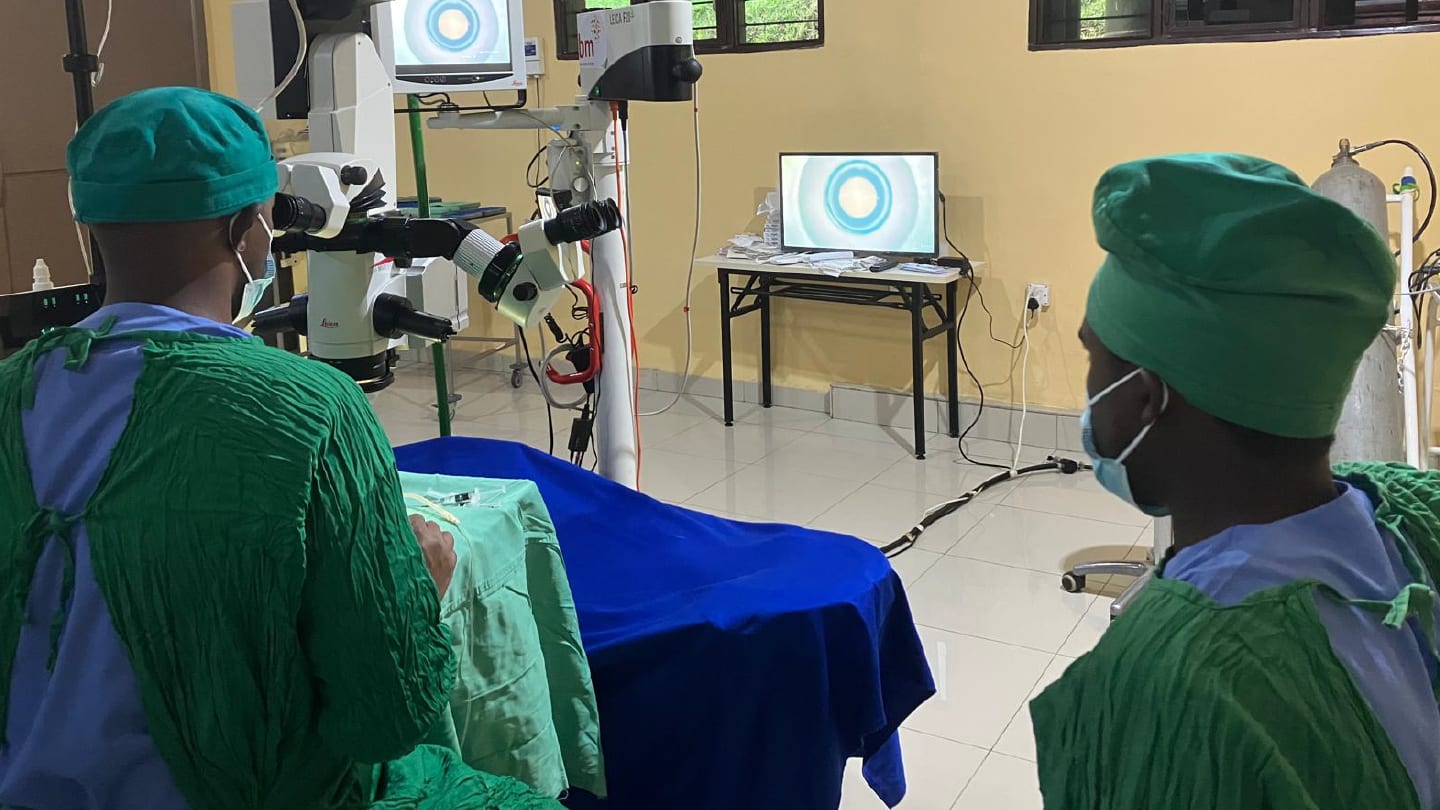
A proof of principle
Our study involved only two surgeons at a single centre, so the results should be interpreted with caution. Larger programs will be needed to confirm whether this model can be reproduced elsewhere.
Nevertheless, our experience offers an encouraging proof of principle.
With the right infrastructure, mentorship, and surgical support systems, advanced ophthalmic surgery can be taught effectively in sub-Saharan Africa. Intensive training programs may help accelerate the development of surgical capacity – but they must be supported by a broader ecosystem that includes ongoing mentorship and access to vitreoretinal care.
The aim is not simply to teach phacoemulsification. It is to build a safe surgical environment where African ophthalmologists can expand their surgical repertoire, gain confidence in advanced techniques, and train the next generation, all with the ultimate aim of protecting patients and enhancing their visual outcomes.
References
- MA Mikhail et al., “Intensive phacoemulsification training in Rwanda: Surgical outcomes of a structured training programme,” AJO International, 3, 2 (2026).
- NC Wong, “The 10 000-hour rule,” CUAJ, 9, 299 (2015). PMID: 26644801.
