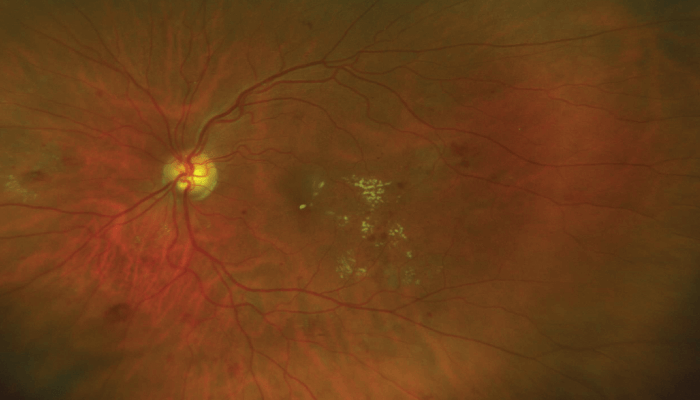
Diabetes has its own unique way of presenting itself to patients – or not presenting itself, as is often the case with this silent disease. Unlike so many other illnesses, where a patient suffers a symptom and seeks help from a doctor – diabetes often does not give the patient any such clues. Think about it: macular exudates, occluded coronary arteries, severe proteinuria, even neuropathic ulcers – more often than not, they do not “announce” themselves to the patient in the typical way. And so, the medical approach has been to identify early signs of complications and then provide treatment that reduces the risk of progression of serious organ damage, which not only shortens life, but also reduces the quality of life.
Screening for diabetic retinopathy (DR) has been shown to be particularly useful in identifying early disease, and, in turn, has allowed early referrals and treatment to reduce the number of people going blind from diabetes. Although it is possible that such a service could be outsourced to smartphones in the future, all solutions appear to suffer a disconnect between the disease pathology or easily measured signal (a raised blood glucose or blood pressure) and the organ damage (DR). And that is true of most of the complications of diabetes. Once a referral is made to a specialist eye unit, doctors do try and include associated specialists, but the nature of specialist medicine is that it is rare for ophthalmologists and diabetologists to be discussing a patient jointly in a clinic environment – even in private clinics, such as The London Diabetes Centre, where they are in the same building and can work together.
So how does the referral process inform the patient? The screening test detects an abnormality and a referral is made. The patient is confronted with words they may not understand; “background retinopathy” is the most common, and the patient fears the worst: blindness. They are not informed of the treatment options; this discussion often does not occur until they see a consultant ophthalmologist. The ophthalmologist has the job – often confronted with information that suggests sight-threatening changes – of telling the patient that they require either laser photocoagulation or intravitreal injections. Explanations of what these do, their potential side effects, how procedures are performed, and what their vision will be like later on – all of these conversations must happen in a limited time, in a busy clinic. It’s therefore likely that these conversations never happen or are rushed.
In this article, I wanted to present the opinions of a patient and retinal specialist to see if there are knowledge gaps in the treatment of DR – ones that can cause patients discomfort or even fear. Should the diabetologist be more involved? In the National Health Service in the UK, once general screening identifies a problem, an appointment is made directly with the ophthalmology department – GPs do not have time for counselling on intravitreal injections, nor do they have the expertise. Is there a role for educational videos to help better inform patients before their appointment?
In my clinical practice, I have the luxury of seeing fundus photographs of my patients on the screen in my room during consultations. It is one benefit of working with a team of ophthalmologists. Many years of clinical contact with patients has taught me that they like to see those changes in their body that signify disease. And they want to receive a relevant interpretation from a specialist. It helps them better understand the course of chronic disease, and aids compliance with therapies. If a patient is shown their fundus photographs every time they attend their diabetes clinic – with a reminder that their blood pressure, glucose and lipid control is key to keeping them out of trouble, they try harder to overcome the problems generated by chronic disease management. And they are better able to cope with recommendations for treatment that may be invasive or destructive. Once I show patients hemorrhages or macular swelling on an OCT image (optical coherence tomography), I have smoothed the process of referral to my retinal specialist colleagues, with a view to treatment being timely and compliant.
We must remember to ask our patients how we are doing. We must deliver not just on outcomes, but also on patient-reported outcomes. Dealing with patient fears and ignorance is an essential role of the modern diabetologist.
Samantha Mann, Consultant Ophthalmologist at Guy’s and St Thomas’ Hospital, and the London Diabetes Centre, London Medical, UK
Diabetic retinopathy (DR) is affected by the systemic control of diabetes. Progression is accelerated if patients have higher sugar levels and uncontrolled blood pressure – and might need a more invasive treatment as a result. It is important therefore that specialists involved in a patient’s care have access to and share information. Not many patients have the luxury of having both the diabetologist and ophthalmologist working together, based on the same site.
In my practice, we offer a screening service, which helps to pick up asymptomatic diabetic eye disease changes quickly and efficiently, which speeds up the treatment, and improves outcomes.
Some patients may only require improvement of systemic control to prevent worsening of their eye changes, but it’s important to develop a realistic management plan with the diabetologist, so that this is not done too rapidly. This could have the opposite effect and actually cause progression of the maculopathy or retinopathy. If systemic control is not enough to prevent the disease from developing further, laser treatment may be required or in more severe cases of maculopathy, a course of intravitreal injections; this revolutionary treatment allows us now to improve the vision of patients with diabetic maculopathy – something that simply wasn’t possible a few years ago.
Despite its ability to reverse retinal swelling, patients rarely like the idea of having monthly injections in their eyes – and some have a great fear of the procedure. This may help initially to incentivize our patients to try to manage their diabetes better with the assistance of the diabetologist to see if they can, avoid anti-VEGF injections.
If injections are inevitable, I try to explain the process very clearly, talking about the risks and benefits, but also what it is likely to feel like. Once they start the treatment, patients usually see a substantial improvement in vision over the first few months, and can see the reduction of the swelling on their OCT scans when they come back for further treatment.
It is also important to make sure that patients undergo regular eye screenings even if they have good diabetic control and no symptoms, to pick up diabetic changes at the earliest opportunity. Once referred, I also feel it is good practice for the ophthalmologist and the diabetologist to have access to the results including the retinal images and OCT scans to share these with the patient to make them part of the decision-making process. This way the doctors can clearly explain the impact that diabetes control has on the patients’ eyesight, using the images to illustrate the problem.
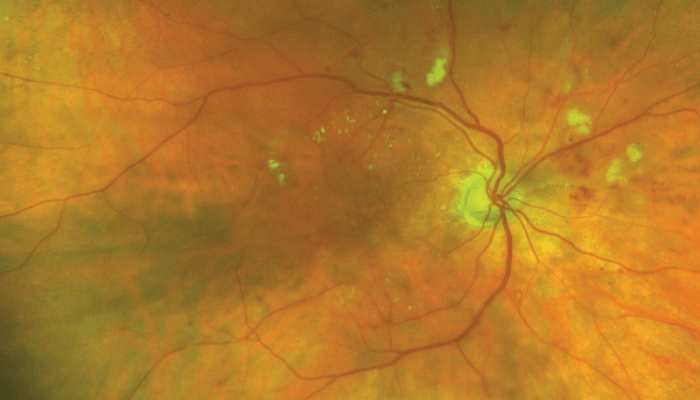
I had gestational diabetes, which went away after my pregnancies, but then I developed type 2 diabetes when I was older.
In public healthcare settings, the care I received was somewhat fragmented, and the way I was informed about the preferred course of treatment for my diabetic eye disease – anti-VEGF injections – was quite abrupt. I was told that it was the only thing I could do not to lose my sight, without a clear explanation of what the process involved. It was quite a scary experience, and I felt a lot of anxiety associated with it.
I decided to change my diabetologist. I met Ralph Abraham, who scanned my eyes, and directed me to the ophthalmologist, Samantha Mann, even though I did not have any ocular symptoms at the time. I have been in their care for two years now, and they guided me step-by-step through the gradual process of managing my diabetes. I got all the information and reassurance I needed before agreeing to a treatment of intravitreal injections. And that meant I felt comfortable and relaxed.
Every time I undergo the treatment, everything is clearly explained. Thanks to the doctor’s attitude, I remain calm and it is a stress-free experience. Based on my experience of different types of setting, it seems to me that, for the patient, it is very important that the diabetologist and ophthalmologist work together in an empathetic way, making the patient feel like their experience is important.
