- Increasing adoption of electronic medical records throughout the NHS provides opportunities to improve outcomes via data analysis
- The RCOphth NOD Audit is capitalizing on this information source to assess cataract patient outcomes per center and per surgeon throughout England and Wales
- By virtue of the richness of these data, the Audit can also employ statistical models to identify high-risk patients, enabling them to be allocated to more experienced surgeons
- Future developments include expansion of the Audit into other parts of the UK and into non-cataract ocular conditions.
We all like to know how well we’re doing – and we are increasingly obliged to ensure that we have that knowledge to hand. Indeed, performance assessment – as measured by patient outcomes – is now a key part of ongoing professional development for surgeons. But measuring performance criteria can be onerous; even a local audit in a representative group of patients is very time consuming, especially if it involves accessing and analyzing hard copies of medical records. Furthermore, medical time is expensive; it just doesn’t make economic sense for each surgeon to spend hours analyzing their own performance.
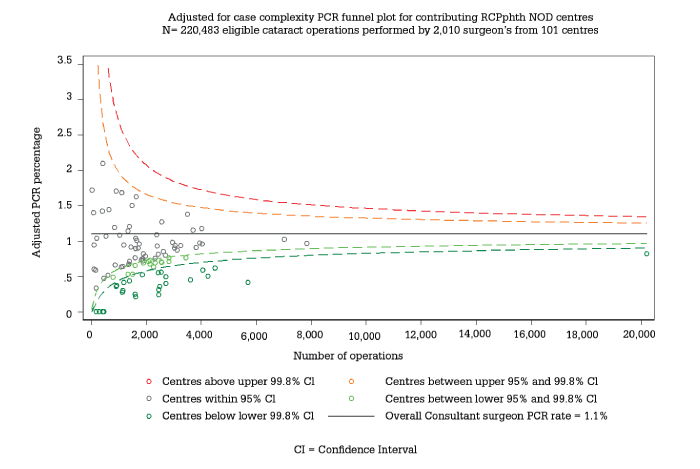
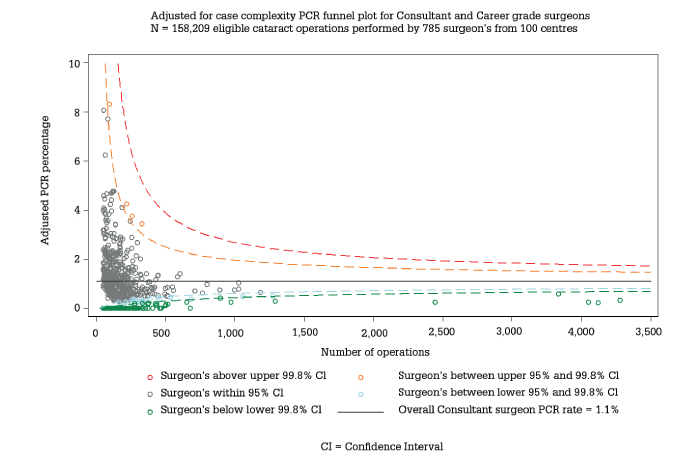
The RCOphth NOD Audit exists to provide performance analysis for ophthalmic surgeons, at least for those who use electronic medical records (EMRs). Obviously, this saves surgeon time – and reduces costs to the NHS – but there is far more to the RCOphth NOD Audit than that. Because we have outcomes data from all over the country, we can present individual surgeon performance measures in the context of peer performance; understanding comparative positioning can be very informative. At the same time, we provide richer analysis, resulting in more accurate appraisal: in particular, we can allow for risk when assessing surgical outcomes. For example, if a surgeon’s case-list is skewed towards complex, difficult operations, the RCOphth NOD Audit would take account of that by adjusting for the complication risk associated with those patient profiles (see Figure 1). In practice, the adjustment gives credit to surgeons who take on difficult cases, rather than penalize them through an outdated appraisal process that can only record good or bad outcomes. In other words, the RCOphth NOD Audit creates a level playing field.
As the Audit has become better established over the last 10 years, its coverage has increased: our most recent report is based on data from over 100 cataract surgery centers in England and Wales, comprising about 218,000 cataract operations for the reported one year period – which is over half the cataract procedures performed in the targeted geographical area (1). During this period we have seen changes in surgeon behavior, resulting in better outcomes – not least, an almost 40 percent reduction in the overall complication rate from 2010 to 2018, which translates to over 3,000 fewer patients with poor outcomes. In my view, the RCOphth NOD is contributing to this evolutionary improvement, not just by providing excellent retrospective analysis, but also by providing surgeons with informative tools ahead of their procedures. In particular, our calculator facility permits surgeons to enter clinical information about a given patient, and then apply the RCOphth NOD statistical model to obtain an estimate of the predicted complication risk for that particular procedure in that specific patient. This in turn allows high-risk cases to be directed to the most experienced surgeons, while more straightforward cases can be allocated to the trainees. And that’s the true power of the Audit; it focuses minds, and makes surgeons more aware of the need to be very careful in certain high-risk cases. Ultimately, the Audit benefits patients, which is what makes our work so important.
To date, the Audit has focused on cataract surgery outcomes, but the plan is to extend our analysis to other conditions, with an initial focus on areas that practicing ophthalmologists have told us are most important to them. In general, for those hospitals that use EMR systems, we would be able to analyze and report on other procedures just as we do for cataract surgery; you could say our cataract surgery audit is a proof of concept.
In fact, we have already taken the first steps towards broadening our remit: namely, feasibility studies on the application of our methodology to age-related macular degeneration, glaucoma, diabetic retinopathy and retinal detachment surgery. Some of these reports are freely available on the NOD website (2). We will first focus on AMD. Why? It’s high volume, very expensive, and extremely important to patients and healthcare providers alike. And consider this: the UK NHS spends an estimated £500 million per year on AMD drugs – and doesn’t know what the outcomes are! That is clearly unacceptable; unfortunately, the NHS prefers not to fund a RCOphth NOD AMD audit at present, despite our proven ability to implement this kind of outcomes analysis. Perhaps that’s a reflection of the current budgetary environment.
Glaucoma is another area I’d really like to target, not least because it happens to be a particular interest of mine. But this will be a challenging condition to include in the Audit – unlike cataracts, where treatment periods are relatively short, glaucoma is lifelong, and its management goes on for extended periods, typically 15 to 20 years. And that means each patient is likely to have significant hospital records – and, very often, much of those records will be in paper form. Just to enter all that information into an EMR would be a significant task – a point illustrated by our pilot study on auditing glaucoma treatment via the RCOphth NOD. We looked at the single measure of visual field preservation among patients attending five glaucoma centers, and found that it was possible to link clinical data with relevant visual field outcomes, but that there were issues with regard to IT implementation and to getting older medical records entered into the EMR. We concluded that a comprehensive RCOphth NOD Audit for vision preservation in glaucoma is not a short- or even medium-term goal – it will take 10 or 20 years.
But the real barrier to the evolution of the Audit is the availability of funding. When we started this initiative, we had no external resource – we were just enthusiasts doing something we thought worth doing. Later on, we attracted some financial support which we used to employ a statistician; we continued to build up our expertise in that piecemeal way until we received five-year funding from the Healthcare Quality Improvement Partnership (HQIP), the intent of which was to get the Audit established. These funds have now run through, so we are looking into other sources of support; for example, from participating centers and lens implant manufacturers. We’ve had encouraging responses from many centers who recognize the benefits of participation in the audit and are willing to pay a subscription, as well as some positive discussions and contributions from lens manufacturers. Furthermore, there might be a benefit to the cessation of HQIP funding in that, in future, we will be able to include Scotland and Northern Ireland in the Audit – we couldn’t do that while in receipt of HQIP monies. So Northern Ireland will be included in the RCOphth NOD from 2020, and we’re planning on how and when to get Scotland to participate too. However, until we get money in the bank, we are in survival mode.
Assuming that funds are not limiting, what does the future hold for the RCOphth NOD Audit? Firstly, I look forward to being able to report on all the cataract surgery being done throughout the UK, including Scotland and Northern Ireland. This wider audit will allow us to provide ever better guidance for surgeons and reassurance for patients – and, I believe, it will enable us to show patients that it doesn’t matter which hospital they choose for their cataract procedure, because all NHS eye surgery departments are doing well. And that, I think, is a very important message. Secondly, I anticipate that expansion into non-cataract conditions, such as AMD – and eventually glaucoma, will enable us to ensure that these patients are also getting the right treatment and the best outcomes.
But regardless of what the future holds, I am delighted with what we have done with the RCOphth NOD Audit to date. We are now international leaders in the ophthalmology auditing field; though I admit this is partly due to our single NHS system, in which many patients are treated in EMR-compliant treatment centers. In these hospitals, therefore, the RCOphth NOD may have access to the entire record of each patient – which provides us with a richness of data that other countries, with other systems, simply cannot match.
Others have started to move in the same direction as the RCOphth NOD – for example, the Intelligent Research in Sight (IRIS) Registry in America – but, I understand, with only mixed success. We in the UK are very fortunate to have a dataset that is both very large and very rich; it’s what enables us to provide unique advantages to ophthalmological services stakeholders, such as adjusting for complexity on a case-by-case basis. No other large-scale audits can offer that kind of benefit.
References
- The Royal College of Ophthalmologists, “National Ophthalmology Database Audit” (2019). Available at: https://bit.ly/2r39GBd. Accessed November 15, 2019.
- The Royal College of Ophthalmologists, “NOD Audit Annual Reports” (2019). Available at: https://bit.ly/2NYkSb4. Accessed November 15, 2019.
- The Royal College of Ophthalmologists, Publications (2012-2019). Available at: https://bit.ly/2OuP4db. Accessed November 15, 2019.
