A seven-year-old presents with −1.25 D of myopia. The refraction is straightforward, the child is doing well in school, and spectacles will provide immediate visual clarity. Yet the consultation raises a more complex question: should myopia control be initiated now?
For clinicians, the evidence supporting interventions that slow axial elongation continues to strengthen (1). However, in practice, treatment decisions are rarely driven by clinical evidence alone. Parents must weigh unfamiliar treatments, uncertain long-term benefits, financial costs, and practical realities of daily life. Their perceptions of risk, safety, and value ultimately determine whether myopia control is initiated.
Understanding how parents make these decisions is central to translating advances in myopia management into meaningful clinical impact, and much of this decision-making is shaped by how parents perceive myopia at the time of diagnosis.

Why parental decision-making matters
Myopia is now firmly established as a major global public health challenge (2), with rising prevalence and well-established associations between axial elongation and sight-threatening complications (3, 4). Critically, the risk of these complications increases in a dose–response manner with increasing myopia (5, 6). Yet these risks typically manifest decades later, creating a disconnect between present intervention and future consequence.
Over the past decade, effective interventions to slow myopia progression have emerged, including low-dose atropine and optical strategies such as orthokeratology, dual-focus contact lenses, and myopia-control spectacle lenses (7-10). Clinical guidelines now clearly recommend that eye care practitioners discuss myopia control strategies with parents of children at risk of progression (11).
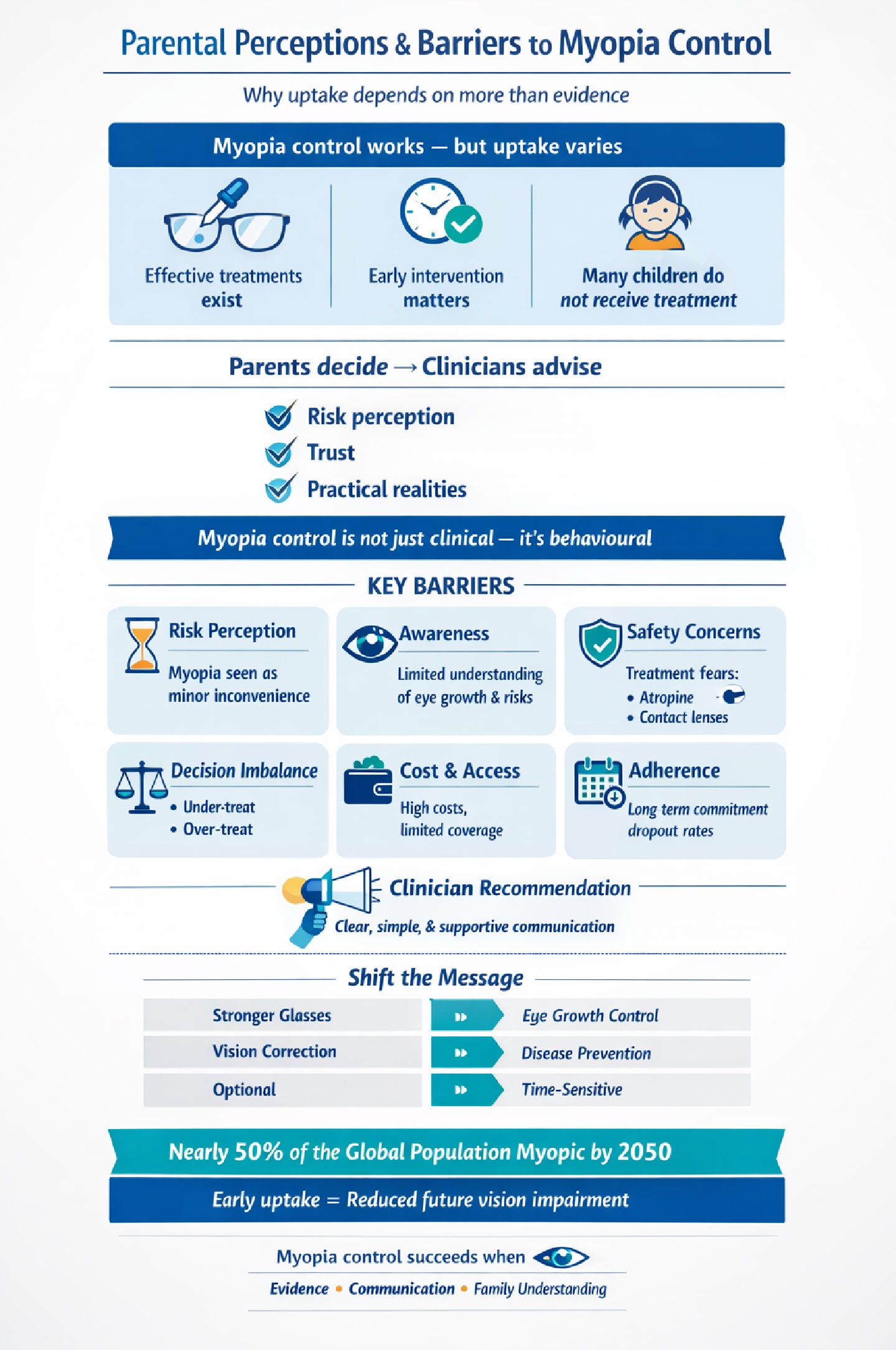
Despite this, uptake of myopia control interventions in clinical practice remains variable (12). In pediatric care, clinicians advise, but it is the parents who ultimately decide. Their perceptions of risk, confidence in treatment, and capacity to sustain long-term management influence both uptake and adherence. As such, myopia control is not solely a clinical issue; it is equally a behavioral and perceptual one, requiring effective communication, shared decision-making, and sustained engagement.
Risk perception: myopia as inconvenience, not disease
A persistent barrier to myopia control is the perception that myopia represents a benign refractive inconvenience rather than a progressive ocular condition (13). Because myopia has historically been framed as a condition easily corrected with spectacles, many parents do not initially recognize the potential long-term ocular risks associated with progressive axial elongation (14). As a result, the rationale for early intervention may not feel compelling, particularly when the child is asymptomatic and functioning well.
This perception is reinforced by the temporal disconnect inherent in myopia: treatment occurs in childhood, whereas complications such as myopic maculopathy or retinal detachment typically arise decades later. For parents, these risks can feel abstract and psychologically distant (15).
Awareness of myopia control options is also variable (13). Many parents are unaware that progression can be modified, while others assume that increasing prescriptions are inevitable or that children may “grow out” of myopia. Collectively, these factors reduce the urgency for intervention.
Parental experience and health literacy
Parental background plays a critical role in shaping decision-making in myopia management (11, 16). Parents who are themselves myopic often have a more intuitive understanding of refractive progression and its potential consequences (15). As such, they may be more receptive to intervention and more willing to invest in treatments with higher perceived efficacy, such as orthokeratology or dual-focus lenses. In contrast, non-myopic parents might ask for more explicit explanations to move beyond the “optical inconvenience” framing.
Health literacy further influences engagement (17-19). Concepts central to myopia control, including axial elongation, dose–response risk, and long-term disease prevention, are not inherently intuitive, particularly within the constraints of a time-limited clinical consultation. Where understanding is limited, decision-making may default to the most familiar, least complex option rather than the most effective.
Importantly, acceptance is only the first step. Sustained adherence over several years requires ongoing motivation, reinforcement, and confidence in the chosen treatment approach.

Beliefs about treatment: efficacy and safety
Even when parents recognize myopia as a progressive condition, uncertainty about treatment can still act as a barrier to uptake (14).
Concerns about treatment safety are a key determinant of decision-making (15, 16). Pharmacological interventions, particularly atropine, may raise concerns regarding long-term use in children, despite evidence from the LAMP (10), MOSAIC (20), and CHAMP (21) trials supporting a favorable safety profile at low concentrations. More broadly, myopia control treatments, especially atropine, are often perceived as pharmacological interventions and therefore carry the typical burden of skepticism associated with drug-based therapies in children. This can reintroduce wider issues of trust in medical advice and scientific evidence, necessitating both robust clinical data and a substantial investment in patient-centered communication. Similarly, contact lens–based interventions can prompt concerns about infection risk, hygiene, and whether younger children can safely manage lens wear (22).
In this context, perceived risk often outweighs the statistical risk. Even a low probability of adverse events may feel unacceptable when weighed against a condition perceived as not immediately harmful.
In practice, parental responses to myopia control often diverge in predictable ways. Some parents underestimate myopia, viewing it as a minor refractive inconvenience and declining intervention despite clear evidence of progression risk. Others overestimate both the risk and the need for intervention, sometimes seeking multiple concurrent therapies when a single evidence-based approach would be sufficient. Both patterns reflect a misalignment between perceived and actual risk, complicating shared decision-making.
A further challenge lies in the preventive nature of myopia control. Unlike conventional refractive correction, these interventions aim to reduce future risk rather than address an immediate deficit. Parents are therefore asked to commit to ongoing treatment for a condition that appears adequately managed with spectacles. Without clear communication, this shift from correction to prevention can be difficult to reconcile.
Practical and psychological barriers to sustained treatment
Beyond beliefs about risk and safety, practical considerations frequently determine real-world uptake and continuation of myopia control.
Cost remains one of the most consistently reported barriers (14). Many interventions involve additional expense and ongoing review, frequently without reimbursement. For families with multiple children or competing financial priorities, this can be decisive, limiting both treatment uptake and continuation.
Practical burden is equally important. Myopia control requires sustained engagement over years, including regular appointments, adherence to treatment protocols, and lifestyle modifications such as increased outdoor time. These demands may not align easily with family routines, school schedules, or a child’s willingness to engage.
Even in clinical trials, discontinuation rates for optical interventions can reach 6–21% per year (23), highlighting the challenge of long-term adherence.
For some families, pharmacological treatments introduce an additional layer of concern related to medicalization and trust. Preventive use of medication in children may prompt broader questions about necessity, long-term effects, and confidence in clinical recommendations. In these cases, trust in the clinician and in the rationale for treatment becomes crucial.
From individual decisions to public health impact
The cumulative impact of individual decisions extends beyond the clinic. With projections indicating that nearly half of the global population may be myopic by 2050 (24), increasing early uptake of myopia control offers a meaningful opportunity to reduce future vision impairment at scale.
Realizing this potential depends not only on the availability of effective interventions, but on their acceptance and sustained use in everyday practice. Parental decision-making therefore represents a key leverage point for public health strategy.
Structured childhood eye-screening programs can support this by enabling early detection, increasing awareness among parents and educators, and facilitating population-level monitoring. In some countries, engagement begins in infancy; for example, in Belgium parents are informed about myopia risk at ages one and two years, alongside guidance on behavioral interventions (25). Aligning clinical care with public health infrastructure will be essential to translate evidence into meaningful population-level outcomes.
The role of clinician communication
If parental perception is the barrier, clinician communication is the intervention.
Practitioner recommendations are among the strongest predictors of myopia control uptake (11). Yet communication remains variable: some parents receive limited information at diagnosis, while others feel overwhelmed by complex explanations or uncertain about how to choose between their available options (14).
Effective communication requires more than presenting evidence; it requires reframing myopia in terms that are meaningful to parents. Clinicians should emphasize that current clinical trial evidence strongly supports myopia management in children, and that early initiation is particularly important, as younger children are likely to derive the greatest effect (9, 26). Explaining axial elongation as structural eye growth, using axial length growth charts rather than simply increasing spectacle power, can shift understanding from correction to disease prevention. Framing treatment as reducing future risk, rather than simply slowing prescription change, further clarifies the rationale.
Behavioral interventions should be positioned as the cornerstone of management. Clear explanation of outdoor time (27), visual habits (28), and lifestyle factors help families understand their central role alongside optical and pharmacological treatments. At the same time, clinicians should emphasize that there is no one-size-fits-all approach; treatment decisions should always be individualized based on a child’s age, lifestyle, and living environment.
Addressing concerns directly is equally important. Discussing safety in practical terms, demonstrating lens handling where appropriate, and acknowledging cost and lifestyle considerations can support informed, realistic decision-making for parents.
Ultimately, successful myopia control depends not only on what is prescribed but on what families can understand, accept, and sustain over time (23). While the science of myopia management continues to advance rapidly, its impact will remain limited unless it aligns with how families perceive risk, value treatment, and navigate everyday life. Bridging this gap between evidence and lived experience remains a central challenge in myopia management.
The European Myopia Network (EMN) is an open educational and scientific initiative that brings together experts from across the majority of European countries (https://myopianetwork.eu/ ). The network conducts innovative research, shares key developments in myopia through curated educational content, and fosters collaboration among clinicians and researchers.
EMN also hosts educational events, including the upcoming Myopia 2026 online meeting on June 5, which is free to attend. Membership, event participation, and all educational materials are provided at no cost. (https://miopia.pl/conference-2026/ )
References
- S Khanal et al., “Childhood Myopia Part I: Contemporary Treatment Options,” Invest Ophthalmol Vis Sci, 66(7):6 (2025).
- MA Bullimore, NA Brennan, “Myopia Control: Why Each Diopter Matters,” Optom Vis Sci, 96(6):463–465 (2019).
- BA Holden et al., “Global Prevalence of Myopia and High Myopia and Temporal Trends from 2000 through 2050,” Ophthalmology, 123(5):1036–1042 (2016).
- DI Flitcroft, “The complex interactions of retinal, optical and environmental factors in myopia aetiology,” Prog Retin Eye Res, 31(6):622–660 (2012).
- M Moore et al., “Global Patterns of Myopia, Age, Sex and Vision Loss: A Comparative Analysis of US and South Korean National Surveys,” Ophthalmol Sci, 101142 (2026).
- JWL Tideman et al., “Association of axial length with risk of uncorrectable visual impairment for Europeans with myopia,” JAMA Ophthalmol, 134(12):1355–1363 (2016).
- J Huang et al., “Efficacy comparison of 16 interventions for myopia control in children: A network meta-analysis,” Ophthalmology, 123(4):697–708 (2016).
- JJ Walline et al., “Interventions to slow progression of myopia in children,” Cochrane Database Syst Rev, (1) (2020).
- MA Bullimore et al., “IMI—Interventions for Controlling Myopia Onset and Progression 2025,” Invest Ophthalmol Vis Sci, 66(12):39 (2025).
- JC Yam et al., “Low-Concentration Atropine for Myopia Progression (LAMP) Study: A Randomized, Double-Blinded, Placebo-Controlled Trial,” Ophthalmology, 126(1):113–124 (2019).
- KL Gifford et al., “IMI – Clinical Management Guidelines Report,” Invest Ophthalmol Vis Sci, 60(3):M184 (2019).
- Y Whayeb et al., “IMI-global trends in myopia management attitudes and strategies in clinical practice–A nine-year review,” Contact Lens Anterior Eye, 102492 (2025).
- S McCrann et al., “Parental attitudes to myopia: a key agent of change for myopia control?,” Ophthalmic Physiol Opt, 38(3):298–308 (2018).
- S Kearney et al., “Perceptions and barriers to accessing myopia management in the UK,” Children, 11(12):1490 (2024).
- A Abou Adela et al., “Knowledge and Awareness of Myopia Among Parents and Teachers…,” Vision, 10(1):11 (2026).
- S Ortiz-Peregrina et al., “Parental awareness of the implications of myopia…,” Ophthalmic Physiol Opt, 43(5):1145–1159 (2023).
- A Ravid-Saffir et al., “Development and validation of a questionnaire…,” Sci Rep, 13(1):13887 (2023).
- S Choi, J Chin, CY Chiu, “Association between health literacy and health-promoting behaviors…,” J Educ Health Promot, 14(1) (2025).
- A Bruce, T Sanders, TA Sheldon, “Qualitative study investigating the perceptions of parents…,” BMJ Paediatr Open, 2(1):e000307 (2018).
- J Loughman et al., “Efficacy and safety of different atropine regimens… MOSAIC trial,” JAMA Ophthalmol, 143(2):134–144 (2025).
- K Zadnik et al., “Efficacy and Safety of 0.01% and 0.02% Atropine…,” JAMA Ophthalmol (2023).
- KM Cavuoto et al., “Multifocal Soft Contact Lenses for the Treatment of Myopia Progression in Children…,” Ophthalmology (2024).
- J Santodomingo-Rubido et al., “Dropout rates among optical interventions for myopia control…,” Contact Lens Anterior Eye, 49(2):102601 (2025).
- BA Holden et al., “Global Prevalence of Myopia…,” Ophthalmology, 123(5):1036–1042 (2016).
- C Hemptinne, N La Grange, D Yüksel, “Vision Screening in Belgian Children…,” Ophthalmic Epidemiol, 27(5):364–375 (2020).
- S Khanal et al., “Childhood Myopia Part I: Contemporary Treatment Options,” Invest Ophthalmol Vis Sci, 66(7) (2025).
- C Lanca et al., “Near work, screen time, outdoor time and myopia…,” Acta Ophthalmol (2021).
- S Marcos, “Optical and Visual Diet in Myopia,” Invest Ophthalmol Vis Sci, 66(7):3 (2025).
