In 2014, Silicon Valley-based entrepreneur Joon Yun launched his $1 million Palo Alto Longevity Prize as an incentive to scientists to fix the “problem” of aging. In nearby Novato, Deepak Lamba’s group at the Buck Institute for Research on Aging have been focusing on fixing this problem (or at least the retinal degenerative disorders associated with aging) with stem cell therapy (1).
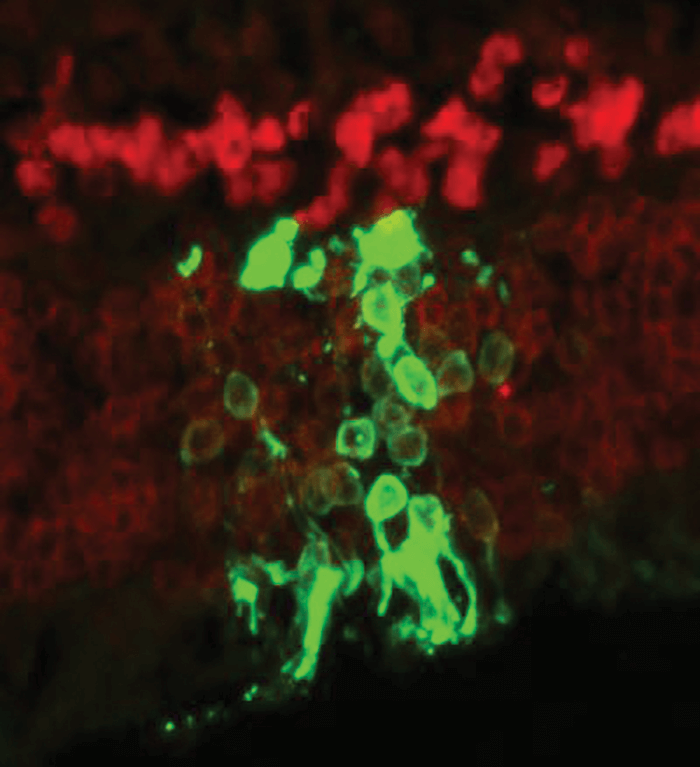
To be efficacious as regenerative therapies, stem cells must be able to live long enough to integrate into the host tissue and “do their job.” Currently, this isn’t always the case; they can be rejected by the immune system shortly after transplantation or fail to thrive in degenerated or diseased tissues. Although Lamba’s group had previously shown that human embryonic stem cell (hESC)-derived photoreceptors transplanted into murine retinas could integrate and function (2), it has been difficult for researchers to demonstrate long-term functionality and restoration of vision. “A major controversy in the field is whether the transplanted photoreceptors simply die off or are actively rejected by the immune system,” says Lamba. To try and settle the matter – and potentially improve stem cell longevity – the team transplanted hESCs into severely immunodeficient interleukin 2 receptor γ chain (IL2rγ) null mice (IL2rγ-/-), which are essentially phenotypically normal, apart from the fact that they can’t reject transplanted cells (1). In such mice, the team found that the number of mature hESC-derived cells that integrated into the retina increased 10-fold (3). They also showed that transplanted hESCs could restore light sensitivity in congenitally blind Crxtvrm65 mice, and that this restoration of visual function was significantly greater in immunodeficient Crxtvrm65/IL2rγ-/- mice at three and nine months post-transplantation than Crxtvrm65/IL2rγ+/+ mice (p<0.001 and p<0.01, respectively) (1).

“We show that these mice can now perceive light as far out as nine months following injection of these cells – that gives us a lot of hope for patients,” says Lamba. The team’s findings suggest that an immune suppression approach might be an effective method of increasing the functional lifespan of stem cells used for photoreceptor replacement therapy and potentially improve clinical outcomes. Lamba notes, “We have found that we can’t ignore cell rejection when trying to transplant stem cells into the eye.”
References
- J Zhu et al., “Immunosuppression via loss of IL2rγ enhances long-term functional integration of hESC-derived photoreceptors in the mouse retina”, Cell Stem Cell, (2016). [ePub ahead of print]. PMID: 28089909. DA Lamba et al., “Transplantation of human embryonic stem cell-derived photoreceptors restores some visual function in Crx-deficient mice”, Cell Stem Cell, 4, 73–79 (2009). PMID: 19128794. Buck Institute for Research on Aging, “Improving the longevity of functionally integrated stem cells in regenerative vision therapy”, (2017). Available at: bit.ly/BuckRelease. Accessed January 24, 2017.
