With Anthony Khawaja, Consultant Ophthalmologist at Moorfields Eye Hospital and UCL Institute of Ophthalmology, London, UK
Louis Pasquale, Site Chair of the Department of Ophthalmology at Mount Sinai Hospital, New York City, USA
Ellie Chabi, Vice President of R&D for the Glaucoma and Neuroprotection Therapeutic Area, Santen
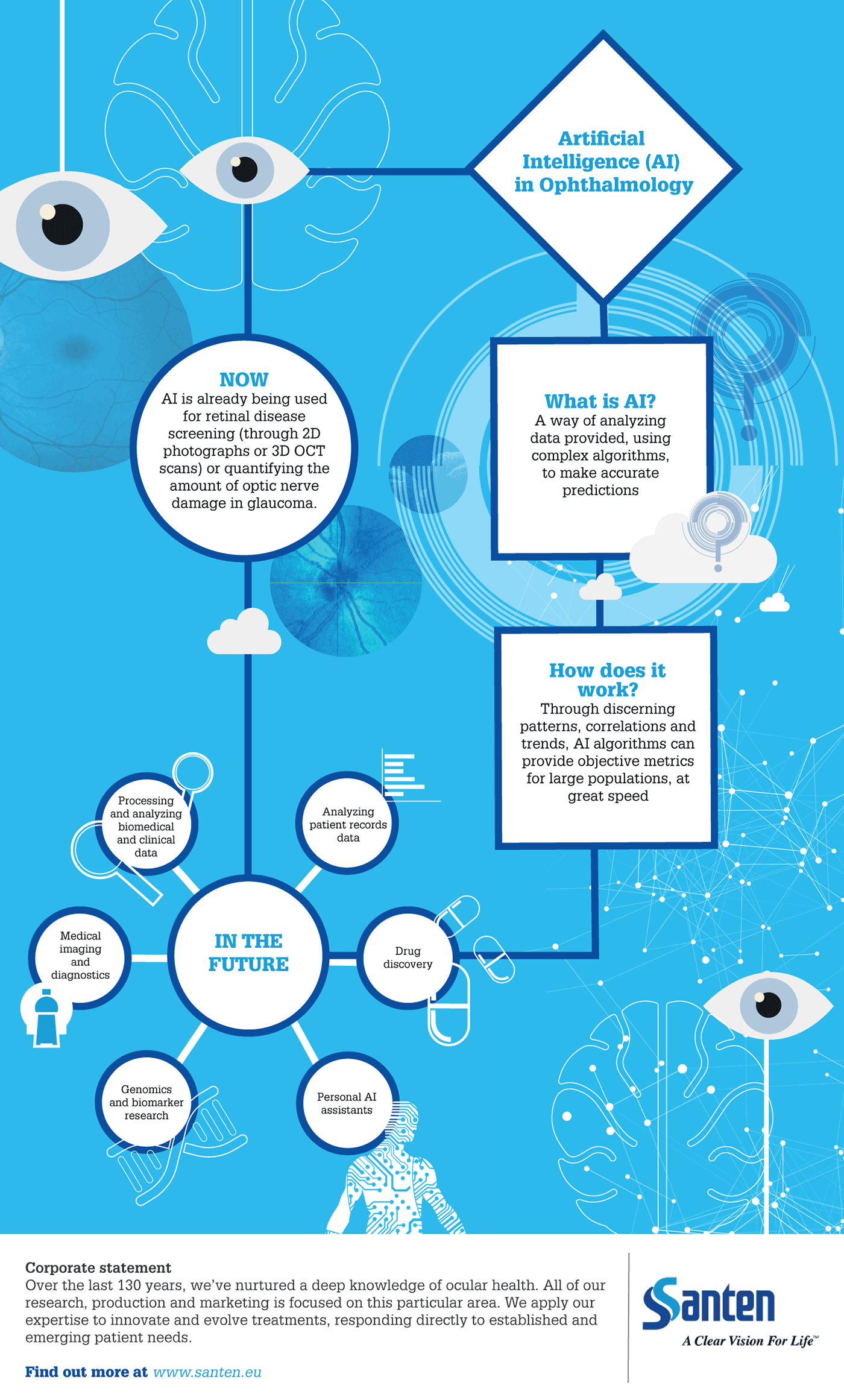
Artificial intelligence (AI), “big data,” block-chain and edge computing are all ways of collecting, storing and analyzing information that, if leveraged effectively, have the potential to rapidly speed up progress in healthcare. AI, with its ability to discern patterns, correlations and trends in huge volumes of data, is among a swathe of new technologies that experts expect to have deep, revolutionary impacts across numerous sectors. Already, ophthalmologists have shown that AI algorithms can provide objective metrics, from simple photographs and optical coherence tomography (OCT), as well as quantify the amount of optic nerve damage in glaucoma. Given the speed at which AI is able to accurately work, many experts predict it will help alleviate time and resource pressures against the backdrop of an aging population – a particularly pertinent issue, given the shortage of ophthalmologists.
Though research and integration of AI in healthcare is ongoing, it has the potential to transform a number of areas – including processing and analyzing biomedical, clinical and patient data; medical imaging and diagnostics; drug discovery; biomarker research; personal AI assistants; and genomics. There is also a wealth of AI research underway in retinal disease, notably the Moorfields and Deepmind collaboration – a project that is investigating the use of AI to read complex eye scans and detect more than 50 eye conditions, and identify patients who require urgent treatment.
Anthony Khawaja, a Consultant Ophthalmologist at Moorfields Eye Hospital explains how the project came about. “The collaboration was initially in the field of retinal disease: reading macular OCT scans to decide whether a referral needs to be seen urgently, routinely, or not at all. It was exciting work that received a lot of attention in the scientific and lay press.” So successful, in fact, that the team has expanded its scope to look at glaucoma. “Glaucoma is the second most common cause of blindness in the world. It cannot be reversed or fixed, so it makes sense to identify glaucoma as early as possible – before people have lost a significant amount of vision,” says Khawaja. “But the problem is that glaucoma is hard to diagnose in the early stages and general population screening isn’t currently recommended.”

In a review of currently available technologies, Public Health England found that it would not be cost effective to screen the whole population for the condition, as no test has sufficiently accurate positive predictive value. Other European countries follow similar policies, based on mass screening studies (1). “If we screened everybody in the UK using our current methods, there would be too many unnecessary referrals to secondary care. It would be a waste of resources,” Khawaja explains. So what is the solution? Can modern technologies like AI improve positive predictive value? “I think so,” says Khawaja. “But we’re a long way off from that just yet. Most work being done is based on a fundus photo of the optic disc. In terms of screening, any time you use AI, you need to train it according to a ground truth. All of the training that has been done so far on glaucoma algorithms has aligned with what an ophthalmologist would think using the same photograph as the ground truth.”
For glaucoma, the concept of a “ground truth” is complex. “If you were to show a series of photos to 10 glaucoma specialists, sometimes everyone will agree there is no glaucoma, sometimes they will all agree there is glaucoma, but most of the time, nobody will agree. This is what makes a ground truth so difficult to establish,” he explains. But there is hope. Studies have developed ways of grading what specialists do agree on, and trained computer algorithms to predict whether someone is at risk of developing glaucoma or not. The algorithms do very well, outperforming ophthalmologists who are not glaucoma specialists. “That may sound promising, but it seems – at best – current AI algorithms are only useful in terms of referrals. They don’t appear to reduce false positives or improve the cost effectiveness of screening,” says Khawaja. “In time, it may be possible to train algorithms to pick up referrals, which would provide us with longitudinal data of patients who have received a firm diagnosis of glaucoma and sought treatment. It might be that we can then train algorithms in that ground truth and, ultimately, teach it to identify not only those patients who are glaucoma suspects and require further tests, but those patients who will actually have glaucoma in the future. And that opens up all sorts of possibilities.”
Khawaja has already seen AI integrated into other ophthalmic fields, namely retina. “The striking thing about retina is that they already have an FDA-approved machine-learning algorithm that can screen for diabetic retinopathy (DR) in IDx Technologies, Iowa, USA, developed by Michael Abramoff. To my knowledge, there are no deployed fully autonomous AI systems for glaucoma yet,” he says. “The natural history of DR is well understood. Early studies like ETDRS identified particular features on a fundus photo that clinicians could use to classify patients according to risk of blindness. For example, mild, diabetic non-proliferative retinopathy, severe non-proliferative, proliferative DR – all of which became well-established disease states that prompt certain treatments or levels of monitoring.” Unfortunately, this is where glaucoma differs. “There have been no large natural studies, other than a few placebo ones, into glaucoma disease states, and it is naturally more difficult to diagnose,” explains Khawaja. “Unlike DR, glaucoma cannot be identified by a photo alone – it requires visual field testing, intraocular pressure readings, OCT, and patient history. In some ways, expecting a machine learning algorithm to take over the diagnosis aspect seems more achievable. Before there was a DR algorithm, humans would look at images and grade specific DR features. Once labeled, there would be little disagreement between specialists about the grading of retinopathy. Unfortunately for glaucoma, there are no such hard-cut features, which means there is a lot of disagreement – for example, in terms of optic disc appearances – making it currently impossible to make a diagnosis of glaucoma on the basis of an image alone.”
To get screened for glaucoma, most people in Europe have to visit an optometrist or an optician’s practice. It is in itself, opportunistic, says Khawaja. “If we can get an AI algorithm to screen for glaucoma from a photo, we wouldn’t need an optometrist at all. It would be much more accessible.” AI screening algorithms could be even more beneficial when combined with other technologies. “Imagine a person went for genomic testing and discovered they were at high risk of glaucoma – that could prompt an immediate referral to a specialist, who could then use an AI algorithm to screen for the disease. Combining these technologies may be the key to improving positive predictive value.”
The possibilities of AI are exciting, especially the ability to speed up and streamline diagnosis and reduce the risk of errors – but can it have a similar effect on disease management? Khawaja is optimistic that it can. “Under the current system, every glaucoma patient is treated. In reality, a number of these patients do not need to be treated at all, while some are not treated aggressively enough, leading to irreversible vision loss.” Khawaja provides an example: the UK glaucoma treatment study where people were randomized to receive latanoprost or a placebo (2). Three quarters of the placebo group didn’t measurably deteriorate over two years. Conversely, 15 percent of the people who received latanoprost got worse, meaning that latanoprost alone wasn’t enough for them. “The problem we have now is that it is hard to predict which patients are going to get worse in the future and which ones will not. We hope that this is something that AI can help us with,” says Khawaja. “These ‘superhuman’ algorithms may be able to pick up on patterns too complex for humans to identify, and determine which patients are truly at risk. An exciting example of this is an algorithm developed by the Verily Life Sciences Team, with which Santen has recently partnered, which can predict a patient’s sex from a fundal photograph with 97 percent accuracy. I doubt there is an ophthalmologist who can look at a fundus photo and say with certainty whether it has come from a man or a woman. The fact that a computer can be so strikingly accurate offers some hope that there may be imaging features that can help us better manage patients in the future.”
“A fully autonomous system could reduce the workload for consultant glaucoma specialists and allow them to spend time with more serious patients – for example, those who require surgery or counseling. But even a decision support system would be beneficial, primarily for catching so-called ‘blind spots’,” says Khawaja. “Even though we are well trained as glaucoma specialists, we all have our weak points. If you train an AI algorithm based on the experience of multiple specialists, it won’t have those blind spots.” He gives the example of an ophthalmologist who identifies a patient as low risk and schedules their next appointment for a year’s time. The algorithm is able to pick up on something they have missed and suggest they are seen sooner. It could also work the other way. “If I were to be overcautious, the decision support system might say that, based on data from hundreds of thousands of patients, I can afford to see the patient less frequently, freeing me up to focus on those with the highest risk of going blind.”
Anthony Khawaja considers when we could see AI-based glaucoma management systems integrated into healthcare
Potentially in as little as five years – provided we have the data. The problem with glaucoma is that it is a slow, progressive disease, so trials take a long time. The UK Glaucoma Treatment Study (2), for example, took two years, which is probably how long we would need to assess the efficacy of an AI-suggested outcome. I think it will take a while to get a sufficient level of proof for algorithms of this kind to be commercially available. In five years’ time, I’d like to see prototypes being tested in prospective clinical trials and if successful, subsequently incorporated into hospital management systems. The reward lies in the software’s scalability. The exciting thing is that this software – when it comes – could be deployed widely. If you developed a module that can help identify high-risk patients, you could help prevent unnecessary treatment in low-risk people. The potential impact is enormous.
However, to be able to develop the best possible algorithms, we need data on a high number of patients from diverse populations. There is a real hunger from developers for data to feed into their systems, and I imagine many institutions will find themselves in a position where industry people are keen to collaborate with them because they want that data. It is data that will drive this field forward.
Millions of individuals are affected by glaucoma and, given the aging population, it is a growing public health concern – something that Louis Pasquale, Site Chair of the Department of Ophthalmology at Mount Sinai Hospital in New York City, knows all too well.
Pasquale is currently researching gene–environment interactions in primary open-angle glaucoma. “One of the struggles we have is finding robust, novel environmental risk factors for the disease – I suspect this is because primary open-angle glaucoma is a heterogeneous disease that has many different subtypes.” Pasquale and his team are hoping to discover novel environmental risk factors specific to certain parts of the optic nerve. This regional vulnerability, whereby patients experience damage to particular portions of their visual field, is characteristic of open-angle glaucoma. Pasquale is working on stratifying different categories of early paracentral damage versus peripheral damage using AI. Tobias Elze, Assistant Professor of Ophthalmology at Harvard Medical School, developed a clustering algorithm known as Archetype Analysis that objectively recognizes the different patterns of visual field loss and gives weighting coefficients for each subtype. Pasquale hopes to leverage this algorithm to disentangle the heterogenous nature of primary open angle glaucoma.


The benefits of the algorithm are two-fold: “In addition to being able to objectively stratify fields into regional patterns of loss and quantify the deficits in each of those regions, we believe that the weighting coefficients could be useful for detecting progressive visual field loss,” explains Pasquale, who is already using the algorithm on select glaucoma patients. “The algorithm is ready to be applied now; it’s just that it has not been widely accepted yet. But we’re getting there! I think, over time, people will realize the utility of this method. Do you have functional loss from glaucoma or do you not? Are you progressing or are you not? Our algorithm actually gives you the region in which progression is occurring, as well as the rate of that progression.”
Pasquale has already begun to apply Archetype Analysis to other fields of ophthalmology. “There are pre-existing datasets in neuro-ophthalmology where randomized clinical trials have been done for specific non-glaucomatous optic neuropathies. Patients’ visual fields were collected and analyzed in a reading center, which is a fairly expensive component of conducting a randomized clinical trial. We’re currently using Archetype Analysis to learn the patterns of visual field loss in other conditions, such as idiopathic intracranial hypertension (where pressure builds up in the brain causing compressive optic neuropathy), to see if we arrive at the same conclusions that were previously reported.” The idea being if you can prove you don’t need a visual field reading center because AI can do the same job for less, it will reduce the budget of future randomized clinical trials. But change won’t happen overnight.
Louis Pasquale explains the key barriers to widespread AI adoption
The first barrier is accepting the use of AI systems in healthcare in general, and in ophthalmology in particular.
The second: clinical adaptation. In practice, people can see the potential benefits of AI approaches, but who is going to pay for implementation of these systems? We see this playing out in the USA with the IDX System, an autonomous algorithm for the detection of DR. It took years to develop, it’s brilliant, it works. But is it going to be put into practice? If IDX is used, it may play more of an important role in primary care offices than a retina or general ophthalmology practice because the costs to implement it are high. The average ophthalmologist is probably going to think, “I’m just going to do it the old-fashioned way.” Conversations are going to center around cost, with an ophthalmologist being unwilling to pay for the performance of a task they were trained to do themselves.
The third barrier is proof of generalized ability. We’ve seen spectacular successes for these algorithms, specifically in detection of the glaucoma-like disc, but only in fairly homogeneous populations. Are they going to work in more heterogeneous populations? Personally, I think the answer is yes, but we’re going to need robust proof.
Like Khawaja, Pasquale is realistic about the time frames surrounding AI integration, predicting that they will be dictated by regulatory agencies. “Right now, we only have FDA-approval for DR detection in the USA – but once you get beyond that, there are no approved algorithms for glaucoma .” He gives the example of an internist who can’t get their patient to an eye doctor for DR screening: “It may be less cost prohibitive in those settings than in an ophthalmic practice – I could see it happening in two years.” As for ophthalmic practices, he predicts they will adopt remote monitoring of common complex diseases in the next five years or so. “In other words, if you have glaucoma, you don’t need to come in every four months, you might only need to come in once a year.” If validated remote monitoring systems can be developed, he predicts adoption rates could increase further, as live visits are less than satisfactory for patients – and doctors. “Physicians want to take care of urgent cases because that is what they’re really good at. In the USA, doctors are not yet familiar with reimbursement codes for remote monitoring of chronic disease and haven’t developed any validated systems for such monitoring, but I think they will come in time."
But for the field to progress, we must address some major gaps in glaucoma – namely, the arbitrary target pressures that physicians set to reduce disease progression, says Pasquale. “Josh Stein, a Professor of Ophthalmology and Visual Sciences at the University of Michigan, is using Kalman Filtering [an algorithm used by NASA to guide astronauts to the moon and back] to examine pre-existing randomized clinical trial data with lots of intrinsically embedded visual field data to predict what target intraocular pressures should be.”
Genomics will also have a huge impact on the field, says Pasquale. “We’ve learned about genes associated with primary open-angle glaucoma that produce elevated intraocular pressure. We’re now filling in this genetic architecture such that we could predict which patients will ultimately need surgery. I believe these genetic biomarkers will be part of future AI algorithms, helping us decide if a patient will need more aggressive treatment.”
In addition to screening and diagnosis, AI may also assist with the prediction of glaucoma progression rate, which could help identify those patients with rapid progression who may suffer irreversible visual loss if they are not monitored regularly. With funding from the National Institutes of Health, Duke University School of Medicine is assessing the overall efficacy of brain-computer interfaces (BCI) to detect glaucoma disease progression over time. The researchers, led by Felipe Medeiros, are testing a specific goggle-based device (nGoggle) that presents visual stimuli and uses electroencephalogram to acquire brain signals, with the aim of detecting visual function loss and, ultimately, improving glaucoma assessment. The study is being conducted in partnership with nGoggle Diagnostics, and aims to demonstrate that the BCI can be used for earlier detection of disease progression, leading to prompt intervention and prevention of irreversible functional loss. Products like the nGoggle are dependent on support from industry, who are more than willing to enter the AI-glaucoma space.
In recent years, there have been significant strides in AI development occurring in parallel with advances in computing power and telecommunication as well as increasing quantity of digitized medical records.
Santen has been exploring the range of opportunities for using AI in the drug development process and Ellie Chabi, Vice President of R&D for the Glaucoma and Neuroprotection therapeutic area of Santen, has been a key player in these efforts. Over the past several years, the team has identified a number of areas for potential applications, ranging from more precise subject selection for trials to development of surrogate biomarkers and have already launched projects that incorporate AI development.
Beyond the research realm, Chabi sees the potential of AI to address a number of unmet needs in glaucoma care, including providing better and more ubiquitous screening tools for detection of early stage disease. “In settings where access to ophthalmic care is limited, health care teams could potentially leverage AI and telemedicine to serve as a first-line screening tool and to also triage patients by severity. After diagnosis, such tools could also potentially be deployed to help patients monitor their condition from home almost continuously, thereby serving as an early warning system for any deterioration of their condition,” she explains. Santen has recently partnered with the International Telecommunication Union, a United Nations agency to support “Be He@lthy, Be Mobile” (BHBM), an initiative of the World Health Organisation (WHO) and the ITU, which aim to tackle noncommunicable diseases (NCDs), responsible for almost 70 percent of worldwide deaths. Santen is helping with the mission of using mobile phones and digital devices to raise awareness of the prevention and management of these conditions in ophthalmology.
Though optimistic for the future, like Pasquale and Khawaja, Chabi is uncertain how long it will be before we see a change in patient outcomes as a result of AI. Chabi explains, “The development and practical widespread application of AI to clinical practice would be dependent on many other workstreams and factors, ranging from, for example, legislative (clear and comprehensive privacy protection policies, both nationally and internationally) to financial (compensation and reimbursements to offset investments).” Chabi is “optimistic that over the next decade there will be AI tools with at least some rudimentary capability to predictively classify patients, thereby allowing us to tailor the treatment of those patients with greater precision. Despite the many challenges, in the long-term AI also has the potential to improve access, care, efficiency as well as costs.”
PP-No product-EMEA-0004
Date of preparation: April 2020
References
- K Grødum et al., “A comparison of glaucoma patients identified through mass screening and in routine clinical practice”, 80, 627 (2002). PMID: 12485284.
- DF Garway-Heath et al., “Latanoprost for open-angle glaucoma (UKGTS): a randomized, multicenter, placebo-controlled trial”, Lancet, 385, 1295 (2015). PMID: 25533656.
