
Susceptibility to dry eye disease (DED) increases with age, with a gradual increase from the fifth decade and then a more noticeable increase beyond the eighth decade of life. Incidence of DED increases with an odds ratio of 1.2 times with every 10-year increment, while the prevalence of DED increases between 2.0 percent (self-reporting) and 10.5 percent (Schirmer test score) over a decade, depending on the diagnostic criteria (1). In terms of gender disparity, DED is more prevalent in females; a large population study reported that the prevalence of DED in women increased from 5.7 percent in those under 50 to 9.8 percent in those aged over 75 (2), while in men it increased from 3.9 percent to 7.7 percent within the same age categories (3).
Multifactorial mechanisms of DED
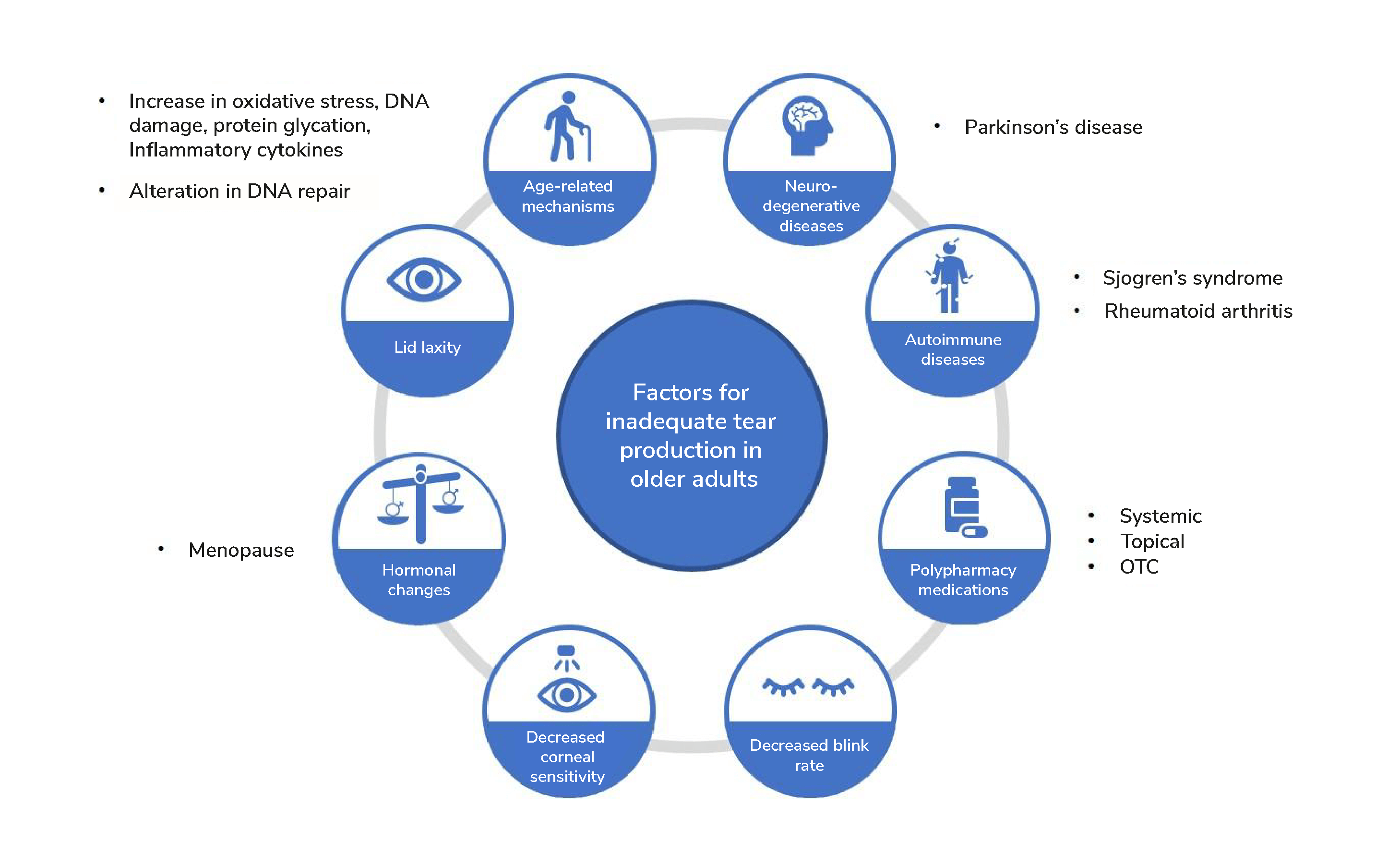
Due to various age-related factors that may contribute to the etiologic mechanisms of DED, such as menopause, Parkinson’s disease, Sjogren’s syndrome, and rheumatoid arthritis (4), older adults are particularly vulnerable to inadequate tear production. Additionally, a higher prevalence of comorbidities in aging individuals – and the medications taken to manage those comorbidities – can also affect the ocular surface.
As people age, the ocular surface becomes more vulnerable to external stimuli, with any diseases or pathological conditions changing the stability and quality of the tear film. Based on multiple extrinsic and intrinsic factors and the underlying mechanisms associated with aging, DED can be categorized into two primary types: aqueous-deficient dry eye and evaporative dry eye. Elderly individuals can be susceptible to both categories – but evaporative DED can occur at the same time as aqueous dry eye.
Meibomian gland dysfunction (MGD) is prevalent among aging patients and is the leading cause of evaporative dry eye. The dysfunction of the meibomian glands is caused by terminal duct obstruction and/or changes in glandular secretion, leading to loss of glands, atrophy, and decreased secretion. The terminal duct obstruction is caused by hyperkeratinization of the duct epithelium and increased viscosity of the meibum (the oily component of tears).
In addition to evaporative DED, this reduced delivery of lipids to the ocular surface can cause hyperosmolarity and tear film instability. Moreover, abnormalities in eyelid position and decreased blinking reflexes, which are common in the elderly, can also decrease tear-film breakup time. In fact, horizontal lid laxity leading to involutional eyelid malposition is a common occurrence, with studies showing that between 50–70 percent of older adults with malpositioned eyelids develop DED (5).
The emergence of the nanoemulsion formulation for DED
The initial treatment for DED typically involves artificial tears to supplement the aqueous component of the tear film. In addition, the standard of care in elderly patients may include cyclosporine, punctal plugs, low-dose steroids, and topical or oral antibiotics, with androgen supplementation to stimulate lacrimal gland function also considered for older women.
Artificial tears are typically buffered solutions that contain aqueous supplements, such as viscosity enhancers, osmotic agents, and antioxidants, as well as inactive agents like buffers, excipients, and electrolytes. Chronic use of the most commonly used preservative in topical ophthalmic preparations, benzalkonium chloride (BAK), has been found to have deleterious effects on the ocular surface, aggravating eye dryness and irritating ocular tissues (6). In light of this research, preservative-free artificial tears may be a better alternative for older patients, especially considering the pathophysiological changes that occur in the cornea of these individuals.
Though most artificial tears provide symptomatic relief for DED, they tend not to treat the underlying pathophysiology of the disease. The ideal artificial tear would have the potential to restore both aqueous and evaporative deficiency. Commercially available lubricant eye drops based on polyethylene glycol/propylene glycol (PEG/PG) in combination with hydroxypropyl guar (HPG) have been shown to provide both immediate relief and extended ocular surface protection for DED. Compared with cellulose derivatives, both PEG and PG have lower viscosity, which provides optimal ocular surface protection and lubrication for healing damaged corneas caused by DED (7). Repeated use of PEG/PG with HPG may also provide additional benefits, such as reduced ocular surface staining, greater convenience, and better tolerance (8).
In recent years, longer ocular retention of artificial tears has been achieved with nanoemulsion formulations. Considered an advanced mode of drug delivery system, nanoemulsions consist of colloidal particulates (10–1000 nm) and aim to overcome the drawbacks associated with conventional systems. These lipid-based lubricant eye drops provide temporary relief to DED symptoms and improve tear film stability.
One lipid-based formulation of PG-HPG features dimyristoyl phosphatidylglycerol, which migrates toward the top of the tear film, fusing with the tear lipids to supplement the gaps developed due to tear film lipid insufficiency. This action replenishes the tear film lipid layer, while mineral oils in the formulation help to support the thickness of the lipid layer (9).
We propose – and the evidence above indicates – that PG-HPG nanoemulsion lubricant eye drops could be considered as a tear replacement solution for aqueous, evaporative, and mixed DED.
A clear understanding of the underlying mechanisms of DED is essential for appropriate intervention. Especially in the case of elderly DED patients, questionnaires should be used to assess individual needs, symptom burden, comorbidities, and the effect on quality of life to drive individualized treatment.
Acknowledgement
Medical writing support was provided by Ashwini Atre, PhD, and Deepak Jha, MPharm, from Indegene.
References
- F Stapleton et al., “TFOS DEWS II Epidemiology Report,” The Ocular Surface, 15, 334 (2017). PMID: 28736337.
- DA Schaumberg et al., “Prevalence of dry eye syndrome among US women,” Am J Ophthalmol., 136, 318 (2003). PMID: 12888056.
- DA Schaumberg et al., “Prevalence of dry eye disease among US men: estimates from the Physicians’ Health Studies,” Arch Ophthalmol., 127, 763 (2009). PMID: 19506195.
- A Sharma, HB Hindman, “Aging: a predisposition to dry eyes,” J Ophthalmol., [Online ahead of print] (2014). PMID: 25197560.
- RW Damasceno et al., “Involutional entropion and ectropion of the lower eyelid: prevalence and associated risk factors in the elderly population,” Ophthalmic Plast Reconstr Surg., 27, 317 (2011). PMID: 21415800.
- K Walsh, L Jones, “The use of preservatives in dry eye drops,” Clin Ophthalmol., 13, 1409 (2019). PMID: 31447543.
- S Srinivasan, V Manoj, “A Decade of Effective Dry Eye Disease Management with Systane Ultra (Polyethylene Glycol/Propylene Glycol with Hydroxypropyl Guar) Lubricant Eye Drops,” Clin Ophthalmol., 15, 2421 (2021). PMID: 34135570.
- M Guillon et al., “Functional visual performance of Systane Ultra after 4 weeks of use,” Investig. Ophthalmol. & Vis. Sci, 52, 3834 (2011).
- L Jones et al., “TFOS DEWS II Management and Therapy Report,” Ocul Surf., 15, 575 (2017). PMID: 28736343.
