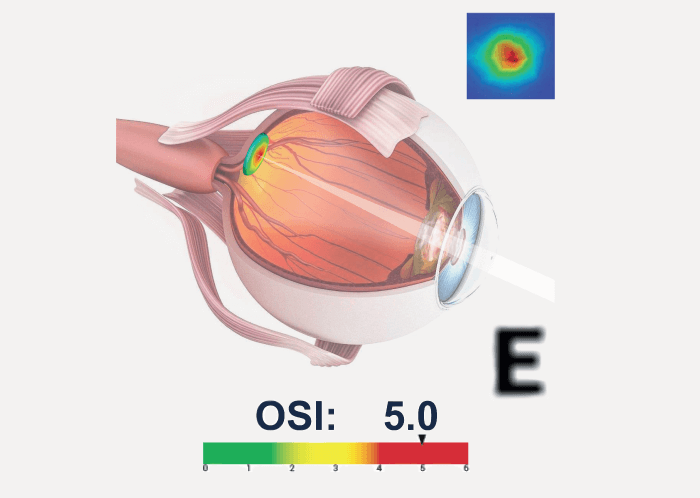
The only way to truly understand your patient’s vision is with the Visiometrics HD Analyzer by Keeler. Built on cutting-edge double-pass technology – the Optical Quality Analysis System – it detects light scatter in the macula and uses it to give an objective measurement of vision quality. Unlike the subjective measurements physicians currently rely on, the Visiometrics HDA offers truly objective results, both pre- and post-surgery.
The benefits of this are threefold. First, it allows physicians to detect early lens changes, ensuring that Lasik procedures are only conducted in patients with no sign of cataract formation. Second, it ensures the best possible decision making for presbyopes in terms of lens or corneal surgery, as well as IOL selection. And that’s important because different IOLs have different vision quality, which is reflected by the Ocular Scatter Index (OSI). With the Visiometrics HD Analyzer, surgeons can confidently manage patient expectations and guide them towards the right procedure and lens. Third, it allows clinicians to measure the impact of tear film in dry eye – not only giving an objective quantification of the patient’s vision, but also a visual illustration to family members of what the patient actually sees. The technology also provides clear evidence to insurance companies, significantly cutting approval times.
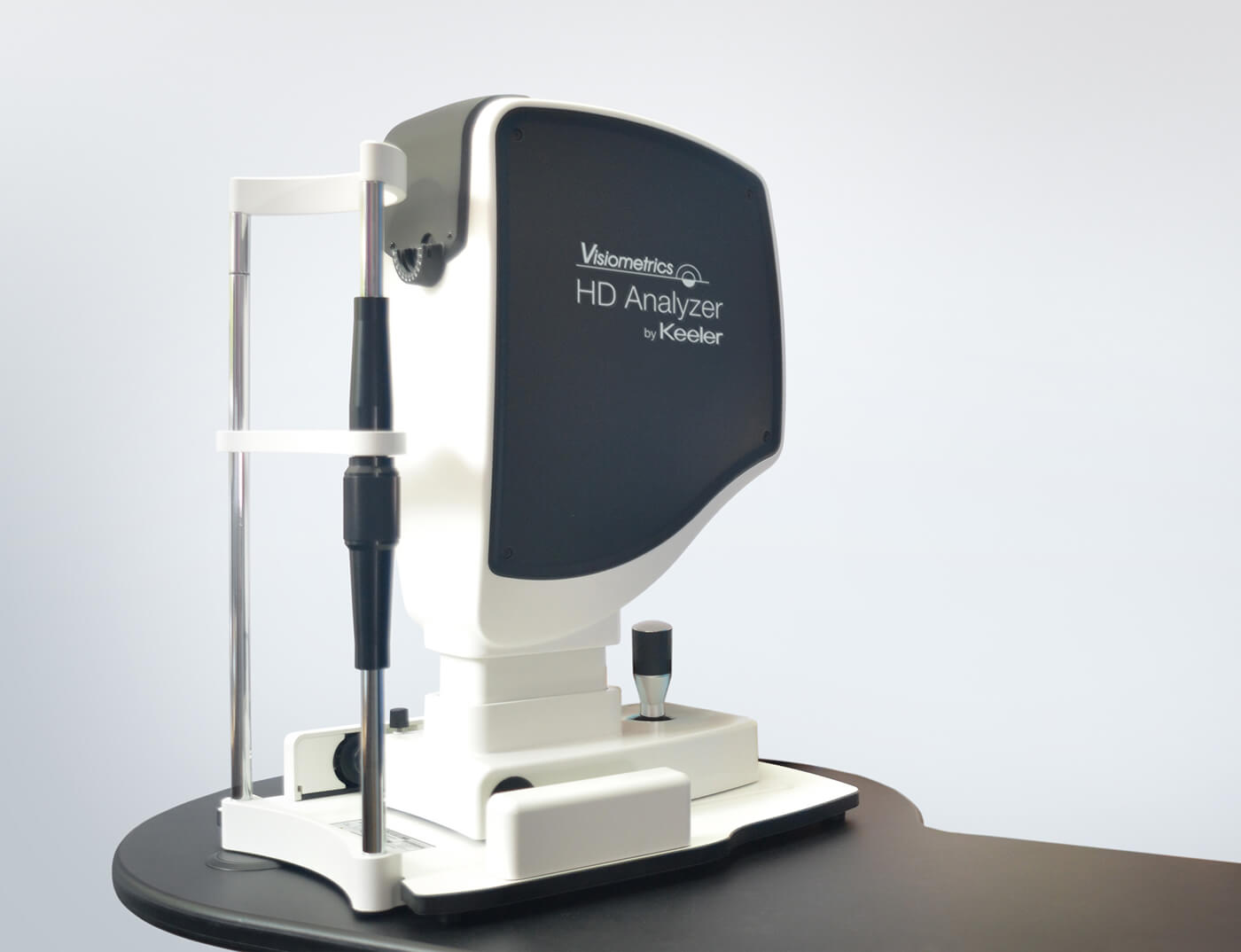
Arthur Cummings, Medical Director at Wellington Eye Clinic, says: “The Visiometrics HDA is my main decision-making device alongside the iTrace device when making a decision on corneal laser surgery versus intraocular surgery.” And it is no wonder – with earlier cataract detection, increased surgical volume, improved conversion rate, reduced chair time and better clinical outcomes guaranteed, it is fast-becoming a physician’s key to diagnostic success.
I’ve been using the Visiometrics HD analyzer for the last three years in my practice for obtaining objective data to assist with tear film assessments. Our practice has a strong refractive focus, and we understand how important tear film is in visual performance – we therefore needed a tool that could help us decide whether the patient is suitable for a multifocal lens or laser vision correction.
If someone comes in for vision correction aged between 50-60 years – and I have no idea what their lens is like from their perspective – then I will always reach for the HD Analyzer. It’s going to provide me with a lot of information about the tear film optical quality, the stability of the tear film and the Meibomian glands. If the lens is clear, but the patient is not seeing well, I can use the HD Analyzer to detect forward scatter – which is the transition of light scattered through the lens, towards their macula. And that gives me a much better idea of what the patient is really seeing, helping me make a more informed decision.
But not only does the HD Analyzer educate me by providing me with all this extra information, it also educates my patients. It allows me to show patients how they are doing with a certain treatment in an objective way. For example, I can use the device to show my dry eye patients exactly what their tear quality looks like. Two images are captured per second, demonstrating how a patient’s blink cycle can vary massively. So just from looking at a screen, you can show patients how the tear film can impact vision. On the optical scatter front, the device also enables the patient to compare an image of what they should be seeing versus what they are seeing. Notably, the patient may actually underestimate the impact of the cataract, because our brains make corrections to improve image quality; nevertheless, the second image is how the cataract is actually degrading vision.
Overall, the HD Analyzer is my main decision-making device when choosing between a lens-based procedure or corneal surgery. And it also helps establish tear film quality in patients being lined up for laser vision correction.

The Visiometrics HD Analyzer has a special place in my refractive practice. We use the device preoperatively for all patients to determine the overall quality of the optical system, and if there is a dry eye component that might be a contributor to a less-than-ideal system. It is also useful in demonstrating to patients that their symptoms are real! Furthermore, I have found it helpful in situations where vision is poor, but the optical system is fine. Here, the HDA provides a level of confidence that the issue is not the visual optics, but perhaps the macula or the optic nerve. Sure enough, further evaluation demonstrates this to be the case.
Probably the most common patients encountered are those who feel their vision is poor – especially at night – and do not look like they have a significant cataract clinically, but the OSI suggests that there are lens changes accounting for symptoms. Post-laser eye surgery patients sometimes have odd complaints about clarity of vision. Again, the Visiometrics HD Analyzer helps break down some of the culprits, which is as useful for my own understanding, as it is for allaying patient anxiety.
The device is also useful in demonstrating early lens changes. Not only does it provide reassurance that a lens replacement procedure is the best way forward, it is equally beneficial in ruling out patients for corneal ablative surgery, as there is no point embarking on a corneal procedure when the lens is becoming problematic. The dry eye assessment, which objectively measures tear break-up by observing changes in the point spread over time, can help identify the cause of the problem, whether that is the ocular surface, the lens or even the vitreous.
Like many surgeons, I like to keep chair time to a minimum. Admittedly, the test – marginally – increases diagnostic time but, importantly, it decreases chair time, as I am more definitive in my decision making. Patients pick up on this, and it improves their confidence in us as a provider. I believe every refractive practice should have access to the HD Analyzer and the many benefits it brings to surgeons – and patients.