Can you tell us who you are and a bit about your professional interests?
My name is Dr Karsten Klabe and I’ve been working in a private practice for seven years. I was formerly the head of the eye department for ten years at the Marien Hospital in Dusseldorf, Germany. I’ve been working as a glaucoma specialist for around 20 years – and as far as I know, I´m one of the earliest adopters of MIGS in the area of North Rhine-Westphalia. After all this time, I’m still interested in introducing new surgical approaches in the field of glaucoma
You’ve recently adopted ELIOS, so can you tell us a bit about it and how it works?
One of the main themes in our office is ‘we love laser’, so ELIOS seemed like a logical progression. We've been using SLT for decades, so adopting a new laser-based approach in the MIGS arena seemed natural. There are important differences between the excimer lasers used in refractive surgery, which uses much shorter wavelengths of light (193nm), compared with ELIOS, which uses an excimer laser with a wavelength of 308nm. This creates the ability to transport the laser energy through an optical fibre to the trabecular meshwork via a specially designed probe. What this means is an excellent safety profile, after all, precise excimer ablation of trabecular meshwork tissues results in no collateral damage to the cornea, or the iris.
Could you describe the ELIOS surgical technique?
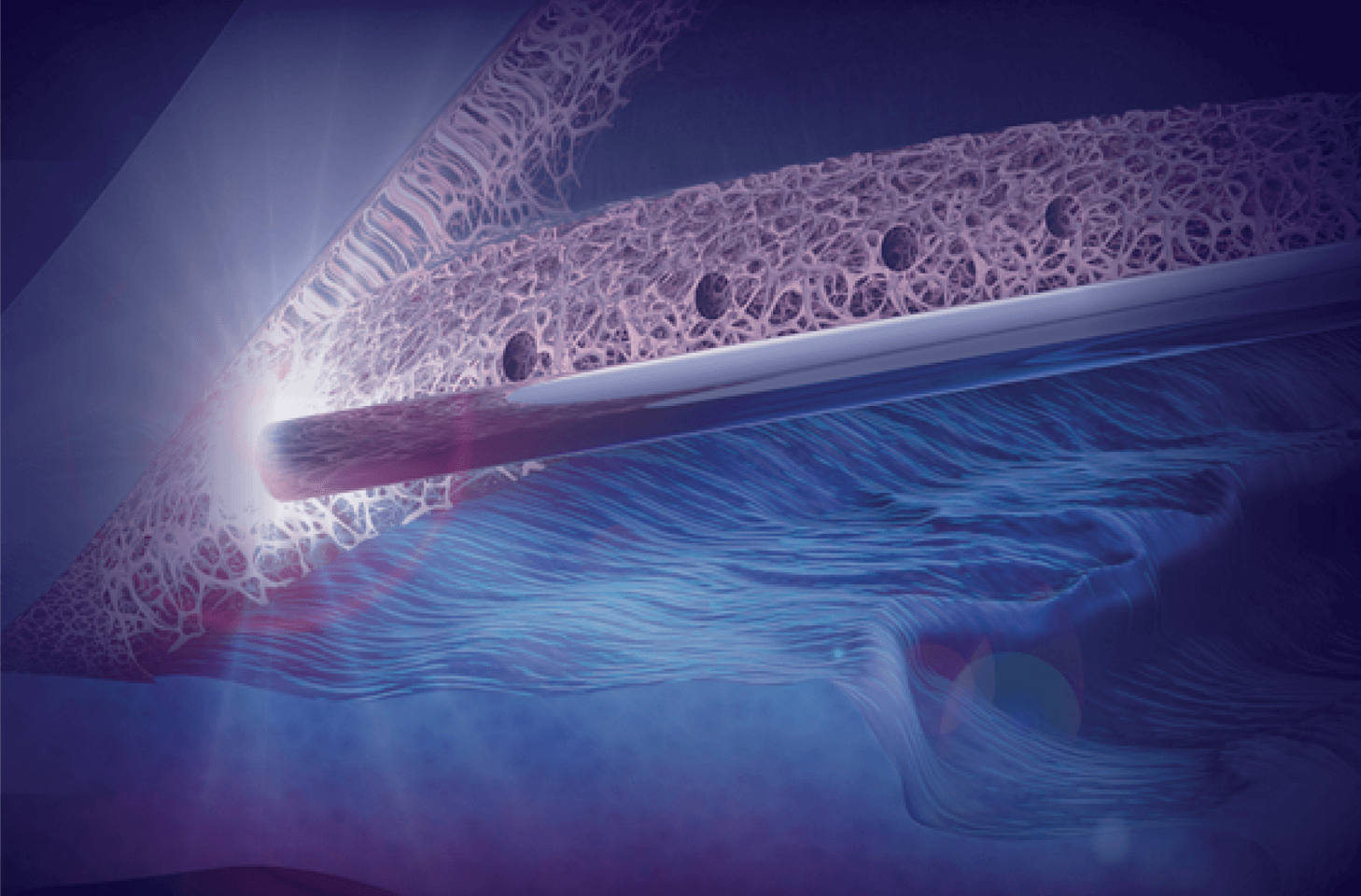
The procedure itself is easy to learn. Under gonioscopic view you introduce a laser probe into the Anterior Chamber, bring the probe in front of the pigmented part of the trabecular meshwork or a part of Schlemm’s canal where blood can be observed. With light contact between the probe and Trabecular Meshwork, depress a foot pedal and create a series of 10 ‘microchannels’, each with a diameter of 210 microns. You typically see a small amount of blood reflux at the site of each microchannel indicating a connection between Schlemm’s Canal and the Anterior Chamber.
We are not short of MIGS options, so where do you see ELIOS fitting in?
We have lots of procedures available to us these days, some with and some without implants. Personally, I prefer the idea of a procedure that does not leave any artificial material inside the eye and that is another reason that makes ELIOS so good. You create 10 microchannels and don’t leave anything behind. There is a high safety profile due to the use of excimer laser energy. It’s a treatment that can be repeated too. You see immediately what happens after ELIOS – with the blood reflux being an indication of success. We routinely offer ELIOS to patients with cataract and coexisting glaucoma with the goal of lowering IOP and stopping medication use after treatment.
What patient characteristics do you look for? What have your experiences been so far?
All that’s required for ELIOS is an open angle. The ELIOS procedure is independent of pigment in the trabecular meshwork compared with ALT/SLT. It’s not only suited to combined cases as it can be performed as a standalone as well. I use it on any patient where the target pressure is not lower than 14mmHg. We know that the percentage of IOP lowering is between 20-40% which fits for around 50% of my patients. I prefer to use ELIOS in patients with 1-2 medications pre-op and pressure not higher than 30mmHg and in my opinion there is a very good opportunity to be medication free after surgery. Previous SLT is not a contraindication for ELIOS as the mechanism of action is completely different. With SLT we are ‘modulating/rejuvenating’ the Trabecular Meshwork but as we know in elderly patients that rejuvenation can be limited. So, even if SLT has been performed previously you will still create the microchannels with the ELIOS excimer laser.
What evidence is available?
Outcomes with ELIOS, formerly referred to as Excimer Laser Trabeculostomy [ELT], have been described in around 16 different publications. We have more long-term data compared with other MIGS devices as we have eight years of data with ELIOS but at best only five years of data with other MIGS devices.
Is ELIOS suited to all ophthalmologists or only glaucoma specialists?
In my hands it is the trabecular bypass procedure with the shortest learning curve, so that’s why it’s not only a procedure for glaucoma specialists. Cataract or anterior segment surgeons experienced with gonioscope guided angle surgery and trabecular meshwork anatomy should take to ELIOS with relative ease.
What should a referral doctor know about ELIOS?
It’s a safe and effective procedure with limited post-op challenges. I haven’t experienced any severe inflammation post-operatively in standalone or combined surgery. We give post-operative steroids for 2-3 weeks followed by NSAIDS for 6 weeks and antibiotics for 1 week. In general, post-op is comparable to post-op care in cataract surgery. You see an immediate effect after surgery, I find that mostly the pressure is down on day 1 at around 12-16mmHg.
Long-term microchannel patency
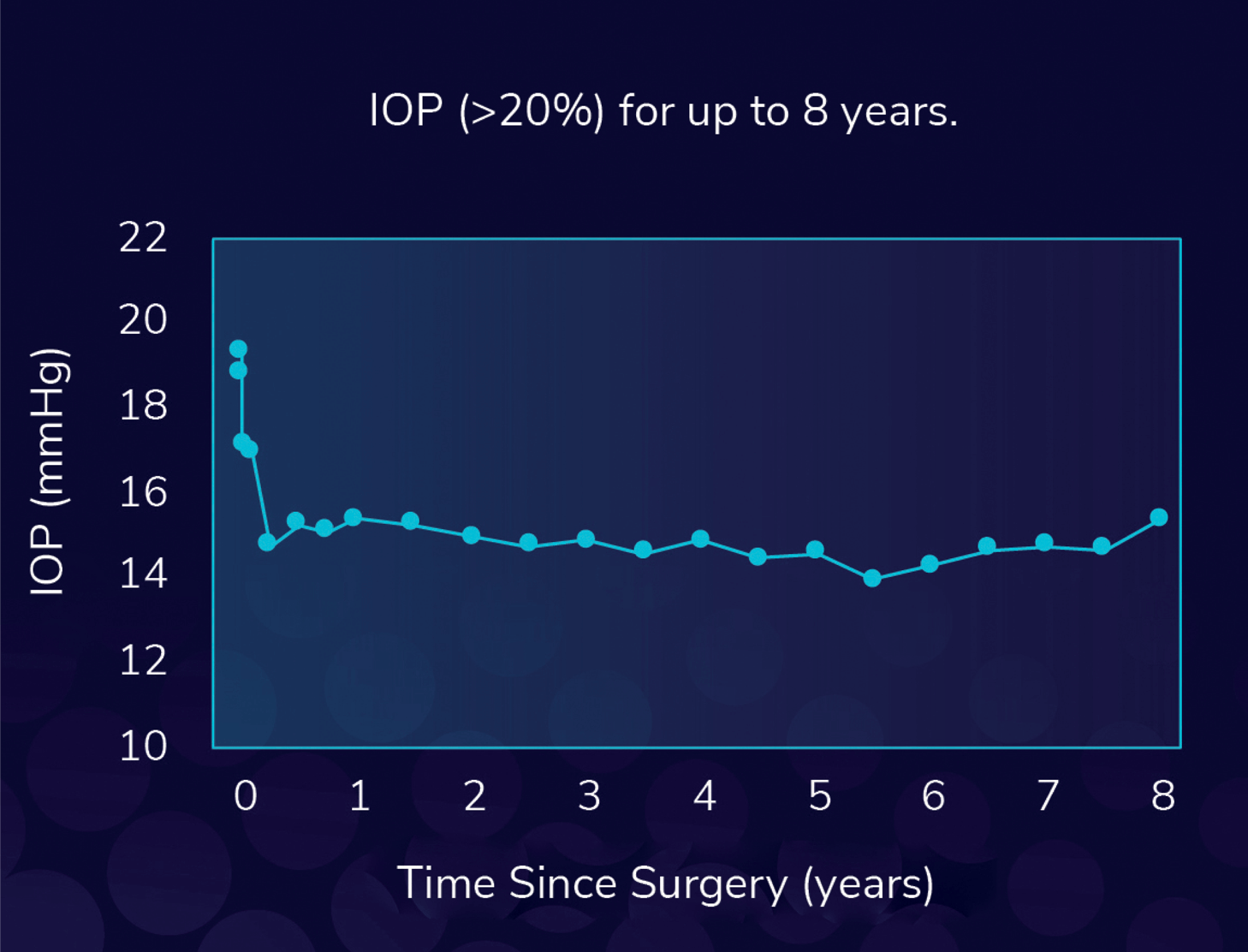
The post-op is very predictable and if needed you can use gonioscopy to examine the superior and inferior nasal quadrant and visualise the microchannels without any collateral damage. Recovery is the same after cataract surgery where after around 1-week patients can return to normal activities.
Disclaimer
ELIOS Vision GmbH is the EU distributor of ELIOS manufactured by MLase AG, located at 82110 Germering, Industriestr. 17 and the FIDO laser applicator manufactured by WEINERT Fiber Optics GmbH, Mittlere-Motsch-Strasse 26, 96515 Sonneberg, Germany. ELIOS is CE marked and licensed for use in the EU in adult patients with glaucoma and is currently under investigational use in the US as part of an ongoing IDE study (FDA). Product feedback should be sent to productsurveillance@eliosvision.com.
The ExTra II (laser class 4) has the brand name ELIOS. The ExTra II is equivalent to ExTra and AIDA devices.