
Why ophthalmology?
As a medical student at Yale, I was required to submit a research paper ahead of my graduation, so the summer after my first year I started looking for an interesting project. I saw a flyer from the ophthalmology department and visited its lab, where I met a group of enthusiastic people who clearly enjoyed what they were doing. It looked like so much fun that I decided that was what I wanted to do.
My second choice was pediatric cardiology – the fellows at Yale were awe-inspiring giants who were saving the lives of tiny babies. However, I realized that I’d have to complete a pediatrics residency, so I chose ophthalmology instead. Nevertheless, I completed a transitional internship, spending a month on a pediatric ward. I remember the chairman bursting into our morning conference one day, asking who had done a lumbar puncture on a newborn the day before. Apparently, no other resident had ever obtained a sample containing no red blood cells, so I suppose I could have also been successful in that field!
Who did you look up to during your training?
I first trained at the Manhattan Eye, Ear & Throat Hospital (MEETH) and was a part of the last group of residents to enter those historic halls as a MEETH resident. My mentors included Jack Dodick, Larry Yannuzzi, Renee Richards, Norman Medow, Richard Lisman, Albert Hornblass, and the inimitable Abe Schlossman. I also spent a little time with Charlie Kelman and heard him give Grand Rounds more than once about his incredible journey and the invention of phacoemulsification. I was very honored to be sitting with his closest friends when he received the American Academy of Ophthalmology’s first lifetime achievement award. To see thousands of ophthalmologists rise as one body to acknowledge his contribution to our field was a truly unforgettable experience.
What’s the biggest change you’ve seen in your subspecialty?
I didn’t truly appreciate it at the time, but I began my training in 1998, which was the time period just after phacoemulsification became widely adopted by most surgeons as the standard of care in cataract surgery. My surgical training was on the Bausch + Lomb Millennium, and we talked a lot about the Venturi versus peristaltic pump systems. Since that time, we have seen many technological advancements with more efficient machines and advanced fluidics, which have made surgery much safer and easier – even for the novice surgeon.
I have noticed this progress most in my surgical teaching. When we first started using torsional phaco, a resident called me about a case I had just supervised, and reported that on post-op day one the cornea was clear. I scoffed and went to examine the patient myself; despite the long phaco time, it was as he described! And that’s when I knew that the new generation of machines was making a big difference.
What’s your proudest achievement?
I spent nearly a dozen years as the Chief of Ophthalmology at Bellevue Hospital, the flagship city hospital in New York City. In this type of setting it is a constant battle for limited resources, and I’d often sit at a table surrounded by chiefs from every other surgical subspecialty – such as orthopedics, neurosurgery, and urology – and they would brush aside our department as being non-essential. I thought: “Hopefully, I will never need their expertise in the future but, as a cataract surgeon, I am sure every single one of them will end up needing mine!” Over the course of my tenure, I managed to convince my colleagues and the hospital administration that sight is an essential aspect of health. We were allocated a marked increase in resources and raised the standard of care to a high level. I am very proud of that achievement.
Please tell us about your humanitarian work...
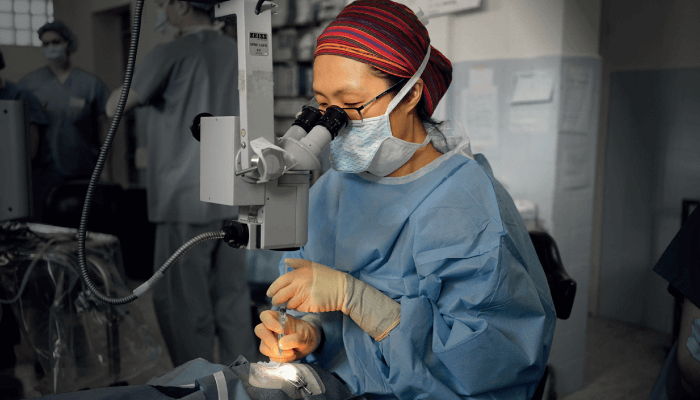
My main humanitarian activities are with the international NGO, Vision Care USA. I have been traveling and performing surgery in east Africa, mostly Ethiopia, since 2013. Through happenstance there are a number of organizations focused on the same region, each with their own area of expertise – the ASCRS Sinskey Eye Institute, the Himalayan Cataract Project, ORBIS/Cybersight, and Sightsavers, among others. All of us share the objective of supporting the development of sustainable eye care systems in this part of the developing world. Vision Care’s niche is the ability to set up and perform portable phaco surgery in addition to MSICS in any part of the world with electricity and clean water. In Ethiopia, we have a partnership with a city hospital in Addis Ababa, and we have been running a Phacoemulsification Training Course (PTC) in collaboration with the Ophthalmological Society of Ethiopia for the last 10 years. I am proud that we have now trained 20 percent of the country’s eye surgeons in modern surgery techniques.
Perhaps even more importantly, we have been able to work collaboratively with many global humanitarian groups, and we’ve seen a synergy and a rise in the fundamental approach to eye care. Global healthcare – and dollars spent on it – usually focus on other needs, such as infectious diseases or maternal and fetal health, but I believe that putting the spotlight on curing world blindness has an exponential impact on global health.
What long-term eye care goals have you been focusing on?
As a faculty member at Columbia University Medical Center, I am serving on a task force to address social determinants of health and the impact of structural racism. The disparity in the delivery of healthcare in the USA needs to be addressed. I believe that the impact of poor vision has been greatly underappreciated in our own neighborhoods. As our population continues to age, ophthalmology will gain an even greater importance in overall healthcare.
What is your ultimate dream for the field?
As a refractive cataract surgeon, curing presbyopia is the holy grail. Though we already have many good tools at our disposal, none of them truly simulates accommodation. There are a few exciting innovations in the pipeline, but my ultimate dream would be a fundamentally radical approach able to reproduce or maintain the eyes of youth.
What advice do you share with your students?
I always begin the academic year by saying: “Remember that what you learn from me now is the cutting edge in terms of surgical technique today, but it is not how you will practice in 20 years. The most important thing is to understand and master the fundamentals – know what the eye is capable of and understand what our current limitations are, so that you will pursue, recognize and adopt future innovations that are worthwhile.” The other piece of advice I give is that, no matter how advanced the technology is, it is not useful if you do not hear and understand a patient’s vision needs and expectations. Listen carefully, and tailor your approach to the individual.
How has the pandemic affected your activities?
We’ve all had to make the shift to telemedicine in the last few months, and I believe this could be a gamechanger for ophthalmology. Even though our department has resumed “normal” clinical activities, I am continuing to work on innovative ways to integrate telemedicine into our clinical practice. One example is asynchronous telemedicine, which has great potential to maximize efficiency in reaching our patients. The use of artificial intelligence to more efficiently triage our patients is also an area of untapped potential; I dream it will, one day, be integrated into our clinical practice.
Because Vision Care’s teams are unable to travel overseas, we are busy converting our Phaco Training Course to a virtual platform. Fortunately, the local doctors we have already trained in Ethiopia will serve as our hands-on trainers, with our remote supervision. We look forward to this innovation in surgical teaching and eagerly await the day we can visit again.
