Much like the Borg in Star Trek, resisting the advance of robots into the operating theater is futile. Their superiority is patent. When operated by a surgeon, they have a number of practical advantages: surgeons no longer need to operate at a surgical microscope – or even in the same room as the patient, dramatically improving ergonomics for them. The robots can filter tremor from the surgeon’s hands – adding years to their effective lifespan as a surgeon. They hold the promise of automating parts of procedures, too – like suturing – saving time and speeding workflow, and they can do things no human can do, like hold a needle in place without movement for extended periods (as required with subretinal stem cell delivery), or scale movement to achieve more precision than a human hand ever could. In fact, we recently reported on the first use of a robotic assistant in man, when Robert MacLaren used Preceyes’ R2D2 robot assistant during retinal surgery to help perform an internal limiting membrane peel (1).

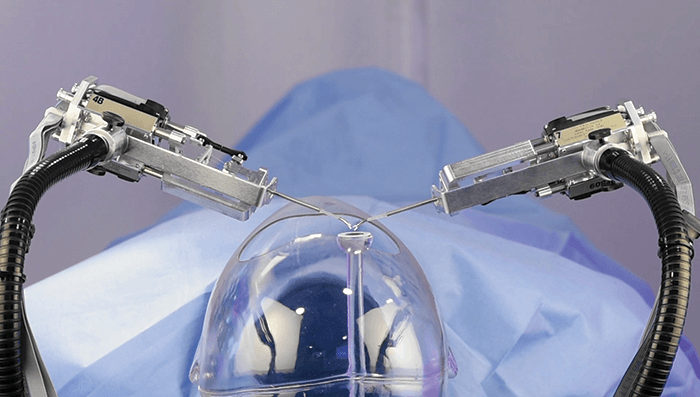
Now there’s another robot on the scene: Cambridge Consultants’ Axsis robot (Figure 1), built to assist surgeons in performing cataract surgery. Chris Wagner, roboticist at Cambridge Consultants in the UK hopes Axsis will demonstrate what’s possible in the next generation of surgical robotics. Here’s what he had to say…
References
- M Hillen, “Forging Iron Man”, The Ophthalmologist, 34, 18–29, (2016). Available at: http://bit.ly/RobotILM.
