
Innovation is rarely a linear process, with periods of rapid advancement often followed by periods of relative stasis. Successful innovation is also rarely driven by technological advancements alone – it is those technological solutions that solve unmet socioeconomic needs that have lasting impact.
The introduction of the Ophthalmoscope (Helmholtz) in 1850 revolutionized ophthalmology (1), and further innovation followed in the late 19th century with the advent of retinal photography, enabling permanent recording and peer review of retinal conditions. Over the following century, one could argue that innovation was relatively flat, with fundus photography and ophthalmoscopy playing a central role in fundus examination and the qualitative determination of patient retinal health.
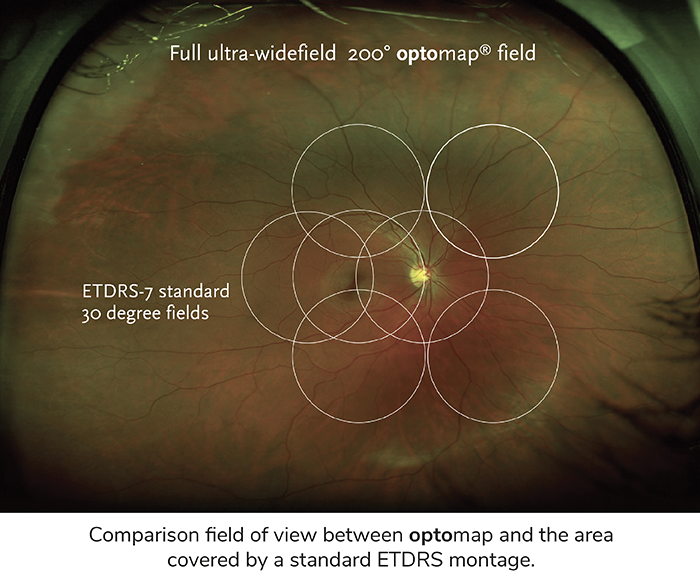
Over the last 30 years, we have again seen a significant acceleration of technical innovation in ophthalmology, providing solutions to unmet clinical needs. The introduction of ultra-widefield (UWF), non-mydriatic, digital imaging overcame limitations in traditional fundus imaging to provide practitioners with tools to detect early signs of retinal disease more effectively and efficiently.
A rapid period of improvement in early UWF imaging, along with the introduction of additional UWF modalities (fluorescein angiography, indocyanine green angiography, and fundus autofluorescence) further enhanced the practitioner’s toolkit, providing deeper insight into retinal health, retinal and systemic disease, treatment planning and patient management. In the same period, we have seen the introduction and rapid uptake of ophthalmic optical coherence tomography (OCT), providing visualization of the retinal and anterior chamber structures and, importantly, quantitative assessment of ocular anomalies and comparison against reference data. This latter point has been the key driver for OCT adoption, playing a pivotal role in the determination of treatment need and monitoring of treatment impact.
Both UWF imaging and OCT have served to overcome specific challenges around disease detection and patient management and, in so doing, have created new challenges and opportunities. We are now at a point of generating significant amounts of ophthalmic image data via increasingly complex and sophisticated medical devices. The output of these devices, especially in the quantitative assessment of retinal anomalies, is not always wholly compatible. We have global healthcare systems under increasing demand from a growing population of elderly patients and an increased prevalence of eye disorders. At the same time, we are seeing incredible advances in treatment, which require validation, monitoring of treatment response, and ongoing management of disease progression. Without the means to manage this complex healthcare data and produce useful guidance within healthcare decision processes, the potential impact of technological advances may be frustrated.
Again, this synergy between the need for technological advancements and the needs in healthcare management has the potential to revolutionize the way in which eye conditions (and wider systemic issues) are detected, managed and treated.

AI in Ophthalmic Care
John McCarthy, emeritus Professor at Stanford, first coined the term “artificial intelligence,” describing AI as “the science and engineering of making intelligent machines.” In other words, computer systems that are capable of performing tasks that can include decision-making, object classification, or the solving of complex problems that rely on the intake and processing of multiple information sources.
Ophthalmology, and healthcare in general, has already moved beyond qualitative image review as a means of detecting and managing disease. Algorithmic and computer vision techniques are routinely used to improve the visualization of specific features, or to provide segmentation of features in medical images. However, interpretation of multiple data sources, determination of prognosis or risk, and workflow management in complex data systems remain limited.
AI has already emerged as a transformative technology in a broad range of fields and applications. In healthcare and, specifically, Ophthalmology, it may offer more efficient and accurate diagnostics, personalized medicine and treatment plans, and ultimately improved patient outcomes. The most obvious application of AI in Ophthalmology is in diagnostic interpretation or disease detection in medical images. AI solutions can be readily deployed to analyze bulk ophthalmic image data with incredible speed to identify anomalies or subtle changes that may be challenging or onerous for a human reader, potentially providing greater consistency in the early detection of disease, vital for timely intervention and prevention of sight loss.
Beyond diagnostics, personalized medicine is becoming increasingly important in the management of both patient outcomes and healthcare economics. Here, AI may play a pivotal role. By analyzing multiple healthcare data points, such as patient demographics, lifestyle factors, image data and previous responses to treatments, AI may help ophthalmology professionals determine the most effective approach to managing eye conditions, and tailoring patient treatment pathways. This may offer benefits in improving patient response to treatments, minimizing adverse effects and optimizing patient interactions with the healthcare system.
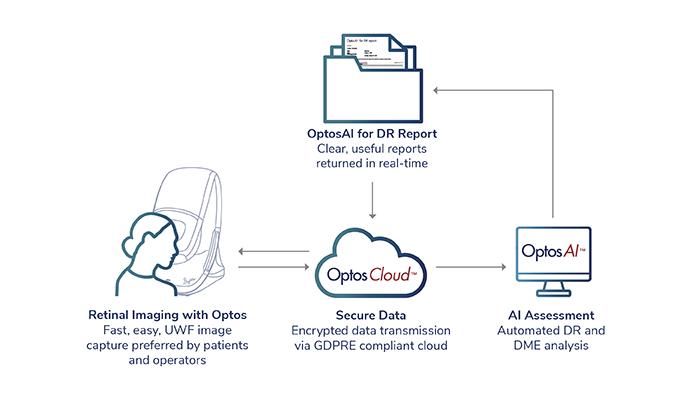
With new advancements in treatment, and the potential role of personalized medicine, we are likely to see an increase in the need for data collection, coupled with a change in the environment in which that data is collected. From hospital to home, telemedicine solutions may offer remote monitoring of eye conditions, powered by AI technologies for the interpretation of image data and management of data and patient flow. Further, telemedicine solutions may also support rural and underserved areas, improving accessibility to Ophthalmic care. Here, AI has the potential to provide both remote monitoring capabilities and to manage patient flow, minimizing the burden on already overstretched healthcare systems.
Beyond patient-facing benefits, AI also has a potentially disruptive role across the lifecycle of ophthalmic practice. In research, AI can provide analysis of vast datasets, including genetic information, clinical records, and imaging studies, allowing researchers to identify correlations that may otherwise have gone unnoticed or with improved efficiency and reduced costs. This may accelerate the rate of scientific discovery and also expose new understandings of retinal disease mechanisms and treatment responses. At a more operational level, AI may also facilitate the automation of routine tasks in ophthalmic practice. By executing tasks such as image management, data entry, and preliminary analyses, AI may allow ophthalmologists to focus on more complex and personal aspects of patient care. This impact on practice efficiency may also extend to reducing the incidence of human error, ensuring a higher standard of care.
According to Eric Topol, founder and director of the Scripps Research Translational Institute, “AI can provide composite, panoramic views of individual medical data to improve decision-making and avoid errors such as misdiagnosis as well as unnecessary procedures. It can suggest testing, interventions and recommended treatments that are appropriate to their needs” (2).
As outlined, it is in this role that AI has its greatest potential – going beyond feature detection and classification into wider healthcare management, optimizing patient interactions, driving practice efficiency and the rate of research discovery, and supporting healthcare professionals to improve the standard of care while alleviating the significant pressures in global healthcare systems. The use of AI within healthcare settings is not without risk, which may be considered along three lines – firstly, what is the remit of the AI solution? Second, in what environment and with what professional oversight is it being deployed? And third, what level of autonomy will the AI solution have? Further, ensuring the ethical use of patient data, addressing issues of bias, performing real-world validation, and avoiding failed benefits are also key, relying on clear and robust regulatory frameworks.
We are seeing a very rapid advancement of AI capabilities and general deployment – collaboration between technologists, healthcare professionals, and regulatory bodies is imperative to ensure that the full potential of AI in ophthalmology is realized, while safeguarding patients, ensuring ethical standards and avoiding clinical error.
In conclusion, the use of AI in Ophthalmology represents a huge opportunity and a potential shift in the way eye care is delivered. From early diagnostics to personalized treatments, as an enabler for telemedicine, a driver of practice efficiency, and an accelerator for clinical research, AI is likely to reshape the landscape of ophthalmic practice. It is, however, critically important that clinical, technological, and regulatory experts work closely together to fully understand the remit, environment and autonomy afforded to such solutions and to ensure clinical, ethical and performance best-practices.
References
- A Grzybowski, “The Ophthalmologist’s Time Machine: Chapter 4,” The Ophthalmologist (2022). Available at: https://bit.ly/3LUThVU
- EJ Topol, Deep Medicine: How Artificial Intelligence Can Make Healthcare Human Again, 1st Edition, Basic Books, 2019.
