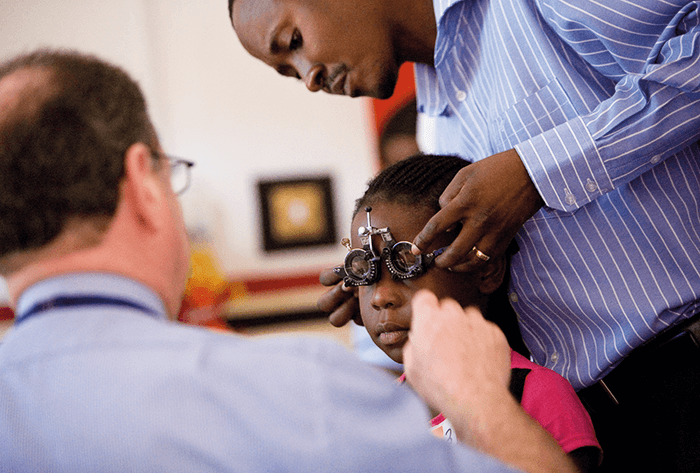
- In part two of our Orbis feature, we meet four volunteers from the organization
- Rob Walters, volunteer surgeon, discusses the focus and priorities of the organization
- Volunteer nurse and global ambassador, Ann-Marie Ablett, shares and reflects on a typical day in a mission, including the need for some fast thinking and a sense of humor
- Luu Tong, a pediatric anesthetist, and her trainer, Andrew Choyce, talk about their journeys and how health education provides many with the ability to train others.
In last month’s issue, we took a tour of Orbis’ new Flying Eye Hospital, and learned about the history of the organization. This month, we feature the stories of just a few of the dedicated volunteers who devote their lives to preventing and treating avoidable blindness and visual impairment across the world. Meet Rob Walters, volunteer surgeon, Ann-Marie Ablett, volunteer nurse and Orbis ambassador, as well as anesthetist trainee and trainer duo Luu Tong and Andrew Choyce. Read about a typical working day with the organization and delve into the unusual practices sometimes required to “get the job done” – like boiling surgical equipment in a wok…
Flying Through Fear
“I realized after day one that I had simply changed location – I was surrounded by different staff and friends I hadn’t met yet” Ann-Marie Ablett, Senior Ophthalmic Nurse at the University Hospital of Wales, Cardiff, Wales, and Volunteer Nurse and Brand Ambassador for Orbis Take us through a typical day with Orbis… We arrive at the aircraft at 7:30 am and change into our “theater blues” and prepare the operating theater – just as we would do at home. Then the surgery begins; we’re allocated different areas by the Lead Nurse and we five nurses take turns overseeing particular programs. We probably perform about five or six surgeries a day depending on the level and skill of the local doctors; our focus is on training, not numbers. We’re there to exchange knowledge and skills so that when we leave the country, the staff will have the necessary skills. After surgery, we hand over care to the recovery nurses, and the patients are then discharged back to the local hospital. After that we have to ‘turn everything round’; we’re nurses by day, but cleaners by night. Sometimes we work until well after 9 pm at night, but that’s part of the charm – no two days are the same. It’s all about the opportunity to transfer and exchange skills.
What kind of skills do you teach? Orbis is incredibly supportive. Before we travel to a country, we’ll be given all the information on the population, culture and beliefs of our colleagues, and also what the specialties will be for that particular program, so that we can prepare. We share best practice on topics such as hand washing as there is a proper way to do it (I remember meeting nurses who had been scrubbing with wooden brushes with hard bristles to ensure they prevented any infection!) We also teach the staff skills such as gowning and gloving, safety and sterility practices (including how to hand the surgeon equipment to avoid needlestick injuries), and how best to advise patients in terms of the expected surgery and possible complications. We cannot guarantee 100 percent – no one can! And also, the importance of hand washing and compliance. In Zambia, the nurses asked what they could do to preserve eyesight. I had never been asked that before, so we spoke about the obvious way to protect your vision and for homework that evening I put a presentation together - luckily I am flexible and have a sense of humor! I prepared a presentation on simple things: best practice with eyedrop medication, safety and protective equipment, getting screened if there is glaucoma in the family, and eating enough greens. All things that we tend to take for granted. I actually learned a lot myself, because I hadn’t thought about how I can protect my own sight – and that makes it a real exchange. How did you get involved? I worked with Rob Walters at the University Hospital of Wales in Cardiff, and, when I heard him talking about Orbis, I asked if I could join! I flew to Chittagong in Bangladesh for my first mission 15 years ago. I didn’t know what to expect. I knew it was hot, but it was hotter than I imagined – and that was just the start of the unexpected! At the hospital, I realized after day one that I had simply changed location – I was surrounded by different staff and friends I hadn’t met yet. I put myself in their shoes, and thought how I’d feel with unfamiliar people coming in and telling me what I’d been doing wrong. But that’s not why we were there; we were there to exchange knowledge and information and we learnt as much as they did. I just asked if they wanted help, and they had a huge willingness to learn. We were readily accepted into the team. And I felt that I was home. Any notable memories? There are so many I wouldn’t know where to start. I remember a young Zambian girl – Mercy – who had slow-to-develop congenital cataracts, and managed to present herself to the doctors when we were in town. She had successful cataract surgery and when we removed the dressings the first thing she did was pick up a book, and she had a huge smile. I only play a small part, but to be lucky enough to be involved in Mercy’s treatment – and her future – is so special; you simply can’t describe it. Many times, we had to think on our feet. In Ethiopia, we needed some tubing to use in a dacryocystorhinostomy but, as is typical in developing countries, equipment was limited. We looked in every room and ended up finding some tubing from an old vitrector. We cut a length and boiled it in a saucepan to sterilize it, then used it to keep the tear duct open during surgery. The procedure was a success. In China, I have seen tubing being sterilized in a wok because the sterilizers stopped working! It’s fair to say that you have to be adaptable and flexible. But, above all, you have to have a sense of humor. I recall one notable surgery where I spent the entire time underneath the operating table holding the plug for the cautery in the socket to stop bleeding! You have to laugh. Who’d have thought that they would be sterilizing tubing in a wok or needing to hold a plug under a table? Nevertheless, those are some of my contributions to care – you don’t know what you’re going to find, but you know you’ll find a way to work around it!
Where to next? Volunteering for Orbis turned out to be one of my better decisions. It has changed my life in ways I never imagined it would, and I’d love to continue working with Orbis for as long as possible. My experiences have been magical. And the old DC-10 aircraft – there was just something healing about it. Some Orbis fairy dust! In 1970, I set out to care for patients – and if I could have the 47 years back, I would do it all again. I absolutely love my job. Do you think you’ll ever go to Arizona to visit the DC-10? Maybe if I am near the West Coast, but it is certainly not on my bucket list because I hate flying! I pray for weeks before we go, feel sick and do not speak to anyone until I land in the country, except to ask for tea! Orbis and my family are the only reasons I’ll get on a plane – the amazing feeling at the end of the trip is worth it – on the way back it’s back to not talking until I land back at Heathrow, knowing I’ll do it all again… Just waiting for the e-mail…
