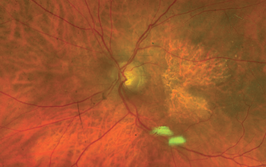
The Stanford Biodesign Fellows
When The Ophthalmologist approached me to tell the story of Oculeve, I first had to explain to them that it all started somewhere odd: heart-rate sensing baby monitors. I was a Biomedical Engineering undergraduate at Vanderbilt University in Nashville, Tennessee, and very interested in the field of electronic medical devices. In my junior year, I started a company with a business student with the intention of making… something. In terms of medical devices, we both knew that we didn’t have the skills to develop something in the regulated medical device field, so we came up with the idea of developing a baby monitor (microphone in one device, speaker in the other) with an additional twist: a heart rate monitor to combat sudden infant death syndrome. If the baby’s heart rate dropped below a certain level, an alarm would go off in the parent’s unit and they could rush in and tend to the child.
The relevance? It was part of the learning experience. We worked on it for a year and a half, until the end of college, and had an absolute ball doing it. But at the end of our days at Vanderbilt, I gained a position in graduate school, my business partner had received an excellent job offer, and we decided to fold the company and move on. But the experience never left me. When I got to graduate school at Case Western Reserve University in Cleveland, Ohio, the environment wasn’t particularly conducive to entrepreneurship (though that has changed since), and that meant I ended up focusing on being a good scientist – and I turned to neuroengineering and neurostimulation.
California Dreamin’!
Next, I headed to Stanford University in California (see Box: Go West!), where I had managed to secure a place on its Biodesign Fellowship Program. And that’s where the Oculeve story really gets going.
The Stanford Biodesign Fellowship is an interesting program. Twelve fellows (eight in my day) are split into teams of four, with each team typically consisting of post-training physicians, scientists and engineers. Teams are normally assigned to a particular clinical area, and for my group, that area was ophthalmology. At the time, all I knew about ophthalmology was that I had two eyes and that they were important to me. What we ended up doing was spending a month in the autumn in the Stanford Ophthalmology clinic, plus a bit of time in local private practices as well, all to observe unmet needs.
Eyeing up unmet needs
Mark Blumenkranz ran the department at the time, and he and the other physicians in the department were immensely generous with their time. We came in, hoped we weren’t too disruptive, and observed their care both in the clinic and in the operating room (OR). When we first got there, we immediately wanted to go into the OR, because you got to wear blue scrubs and feel like a surgeon – we got to ‘play’ doctor for a moment, and we thought that the OR was where the action was going to be. Over that month, our team identified 350 unmet needs – but few were identified in the OR; most were in the clinic. Why? Mostly because the patients in the OR already had solutions to their problems – surgery. We did identify some things that might improve efficiencies in OR workflow and so on, but the clinic was the area that seemed to have the greatest unmet needs. Even in my first week, I’d noticed that irrespective of whether it was the retina clinic, the glaucoma clinic, or whether it was a primary or secondary diagnosis, huge swathes of people coming into these clinics suffered from dry eye – it seemed like it was every third patient. When we started talking to the ophthalmologists, they explained that there were a number of options but, in many cases, there wasn’t really something that could help. There was also an emotional aspect: you could tell that the ophthalmologists were frustrated that there were many patients that they couldn’t help as much as they wanted to. The patients still needed a lot of ‘chair time’ and were often very unhappy too.
Ideas and iterations
The next step was essentially brainstorming. We had a room, a whiteboard, pens, and us. No ideas were stupid, they all got put on the board. At the end of the process, we had filled three of the walls with ink – and had come up with a couple of hundred ideas on how to address dry eye. Some were really quite ridiculous, but one by one, we started narrowing them down until we had a few things that were worthy of further investigation. The neurostimulation approach was one of them.
The first neurostimulation idea was a pacemaker-like device for the lacrimal gland, with a lead that ran up through the neck and into the orbit. We were rather pleased with ourselves, and shared the idea with Chris Ta, Stanford’s cornea chief. We told him, “Look, we had this idea…”, showed him a rough prototype, and asked him what he thought. After his blood pressure returned to somewhere in the normal range (fortunately he didn’t pass out), he said: “Yeah, I think you need to try again, and whatever you do, don’t show this to my patients!”
We went back and iterated the concept several times with rough prototypes and feedback from physicians and patients. I think the first time that we started getting some nodding heads was when we came up with the concept of a small injectable pacemaker-like device that would be placed adjacent to the lacrimal glands and pace it. We realized at this point that such a device would be destined for patients with severe dry eye, but that there was a very real chance that it would work, and it was something that could be done in a procedure room in the clinic rather than the OR.
Raising money
For the next year, I incubated the company on Stanford campus and partnered with a couple of new people: a Stanford postdoc by the name of Jim Loudin, a faculty member you might have heard of: Daniel Palanker – and, of course, Mark Blumenkranz. Over the next year, we were able to raise a little bit of money first through business plan competitions – $50,000 or so – before raising $200,000, primarily through a seed investment from venture capital firm Kleiner Perkins Caufield & Byers. We were able to use that capital to pretty quickly get ourselves into the clinic and ultimately raised about $700,000 in seed capital. We hired a small staff of five and we were able to not only do quite a bit of the development for the implantable device, but also get into the clinic by using some off-the-shelf products, namely a percutaneous stimulator used in anesthesia when seeking nerves for nerve block. Using that device, much to our delight, we found that we could stimulate tear production.
I think the idea of neurostimulation – using electricity – was something that was more than a little foreign to ophthalmologists. We needed to perform a small study to demonstrate the safety of the device and, frankly, to demonstrate to ourselves that it was working in the way we hoped it would. I was the very first patient, or rather, a ‘normal’ subject in that particular study.
Go West!
Towards the end of my degree program, I had a dilemma that I just couldn’t answer: do I stay in academia, or go into industry? My PhD mentor allowed me to spend a handful of months at Boston Scientific in Los Angeles, to try and get a sense of how things work in industry. I learned two things for certain: I didn’t want to remain in academia, but I didn’t think I wanted to start working for a big company either.
What really motivated me to move to the West Coast was my now-wife Kjerstin. I met her while in LA, and frankly, I became very motivated to return to the West Coast after completing my studies in Cleveland. So I started looking, and there was a Stanford Biodesign Fellowship program that was not only closer to the woman who I had fallen in love with, but also seemed to be a great match with my interest. And I thought it might actually give me an opportunity to learn how to do things better the next time around with a company.

The Oculeve team.
From prototype to product
Prototyping is fun – especially in the early stages. The overall process takes a lot of time (it is highly iterative, after all), but the feeling that you’re honing the design and materials to a point where you can bring a medical device that could help many can only be described as exciting. We started off by literally pulling things together in the lab and connecting them up – often even making things with tape and cardboard! Computer aided design (CAD) was certainly used later in the process, but we felt that the physical prototypes were appropriate for the early stages of innovation. There’s little point caring about the look and feel of early prototypes: if it’s likely that you’re going to have to make some important changes later on based on what you find, then it doesn’t make a lot of sense to invest a lot of time in the prototype. “Quick and dirty” was the order of the day: we were doing something to get immediate feedback. When we finally had something to show people that got them to nod their heads, it was a little piece of plastic packaging that I’d cut, and given some shape with a small amount of modeling clay.
The professional product design started in earnest in our second year at Stanford. We got lucky. Janusz Kuzma is an incredible mechanical engineer in the implantables space. He’s a Polish Australian who did the design for the very first cochlear implant – and for several generations of them after that. He has been a lead mechanical designer on several products that are now on the market, not just cochlear implants, but the spinal cord stimulators too. Janusz had retired, and moved to Sydney, Australia, with his wife – but then decided that he regretted the decision to retire. I knew him by reputation and a colleague of mine in the neurostimulation space said that he thought Janusz was getting a little bored. Jim Loudin, the postdoc, and I flew out to Sydney and we spent a few days convincing Janusz to join us – and to do so without salary at first (just stock options) until we had some cash to pay him! We were amazingly lucky that he came on board. Thanks to Jim (on the electrical side) and Janusz (on the mechanical side), we were able to develop a beautiful human-quality implantable device in a really short period of time – just over half a year. And the process was a lot of fun.

The Allergen core leadership.
Luck, Link and Letting Go: Lessons Learned from the Oculeve Experience
Be willing to follow the best idea – whether it’s the one you’re working on or not. Making that transition from the implant to the nasal stimulation program wasn’t an easy decision to make. We had invested a lot of time, effort and money into the program by that point. Despite that, letting go was the right decision.
There is an element of luck when it comes to raising money – and part of that is that sometimes you can be lucky when it comes to the investors and their experience in the business. When you accept somebody’s investment, you’re establishing a long-term and influential relationship with someone, their experience and their opinions, not just their capital. Looking back, we were lucky to have the investors we did.
Be like Bill Link. One thing that resonates from him is that he’s a very genuine person – both personally, and in business. He’s courteous and respectful, recognizes the work of everyone within the organization from top to bottom; in short, he treats people right.

Chris, Jim and Janusz.
An about turn led to an acquisition
Before long, we had implanted close to 40 patients, and found first, that the safety was great. The efficacy was also great – in some patients, but not all. Clearly, we had more work ahead – par for the course with medical device development. Another thing we observed was that despite being a unilateral implant, we were getting bilateral tearing. It was clear that it was working through a different mechanism than we had supposed: we were activating a reflex. Jim and I were in Mexico (where the clinical trials were being performed) thinking about how to really maximize this reflex process, when we thought. “Well, you get a lot of tearing through the nose…” We looked at each other and immediately returned to the hotel to start searching patents and the literature. We couldn’t believe that we were the first to think of this. Physiologically, it’s a remarkable concept: you stimulate a point in the nose, it activates the anterior ethmoidal branch of the trigeminal nerve that innervates the lacrimal gland, and you get an increase in tear production. Much of what we’d done had to be torn up and we started again – but it was worth it.
Allergan approached in April 2015. I believe Allergan’s CEO, Brent Saunders, had talked to a number of physicians (including some clinical investigators of ours) at ASCRS that year, and had decided to place a phone call to us about an acquisition. We then had a very difficult decision to make. We were in the process of raising our Series C financing (of around US$30 million) and we were fortunate to be offered some very competitive terms by some of the venture capitalists involved. At that point, we had been very stealthy with regard to what we were doing – we weren’t talking publicly about nasal stimulation, for two reasons. We were trying to get a head start, one, in terms of intellectual property filings, and two, it was such a goofy idea, we wanted to have the data to back it up, so that when people started learning about it, they were presented with hard clinical data, rather than a concept and a CAD render of a device. The dilemma was: if we entered a due diligence process with Allergan, and the deal fell through, then it would put a bit of a black eye in the Oculeve program in terms of raising financing. Allergan and Brent couldn’t have been any classier about it. We explained the situation to them, and they decided very quickly about whether they wanted to move forward with the deal – and promised that if the deal didn’t work out, they would provide financing at the best terms we were offered. It made us feel a lot better dealing with them. Then, for the next two years, essentially, they left our team unencumbered to get on with it. In the areas that they did get involved, almost without exception, it was to add value.
One of the best examples of this was in the clinical development. Allergan has a huge research and development group, and they probably have more dry eye expertise than anywhere else on the planet. Michelle Senchyna (who went on to be the Allergan lead on Clinical Development for TrueTear) did a great job of extending our knowledge of the basic clinical science and helped generate some very compelling clinical data showing that TrueTear activates all three layers of the tear film: mucin, aqueous and meibum. The company also really shaped the commercial plans too – and added a ton of value to the program. At the end of April, the FDA granted Allergan marketing authorization for Oculeve TrueTear. We had made it – both literally and figuratively.
What’s next
While TrueTear’s commercial story is just beginning, my Oculeve story is over. I stepped down from my position at Allergan soon after the marketing authorization, and the first thing I did was take a really long vacation with my family. What’s next, in some respects, is more of the same. I’m joining a small company called Oyster Point Pharma (OPP), as Chairman of the board. OPP was actually a spin-out of Oculeve, and we’re developing a pharmaceutical treatment for dry eye. I’m also working on an earlier-stage drug treatment for blepharitis – it’s far too early to say if this project will have a future, but what I can say is that it’s lots of fun to be back at the earliest stage again. Hopefully this time, I won’t repeat the mistakes I made last time. It’s a hell of a lot of fun and an incredible journey bringing a new treatment to market. I’ve met and worked with some great people, and I can’t imagine doing anything else right now.
D. Michael Ackermann is Chairman of the Board at Oyster Point Pharma, Inc., and formerly the Vice President of Neurostimulation at Allergan, and President and CEO of Oculeve Inc.
Ackermann is joining Oyster Point Pharma as Chairman of the Board. Previously, he was Vice President of Neurostimulation at Allergan and was President and CEO of Oculeve, Inc. He has twelve years of experience in medical technology development in both academic and industrial settings in the fields of ophthalmology, chronic pain and movement disorders. He has numerous patents and peer-reviewed publications