Keeping up with Precision Medicine
How we’re using a specialized next-generation sequencing panel to give ocular cancer patients access to new targeted therapies
Ophthalmology leads the way when it comes to gene therapy and stem cells. But whilst we may be trailblazing in certain fields, in ocular oncology, we’re trailing behind. For the most part, the treatment of ocular and orbital (abbreviated as “ocular”) tumors have not yet benefitted from many of the emerging and established technologies in oncology and other disciplines to personalize medicine – and there has been no exploitation of cancer-causing genetic and epigenetic changes for diagnostics and treatment. For instance, some types of breast cancers can be treated by epidermal growth factor receptor (EGFR) inhibitors, and patients with certain lung cancers can receive anaplastic lymphoma kinase (ALK) inhibitors. These therapies are based on knowing the gene mutations in oncogenes and tumor suppressors, or copy number alterations (too many or too few copies of tumor promoting or protective genes) that drive the growth of the cancer. An emerging field that has deepened our understanding of how tumors form is epigenetics (See “Epigenetics Explained”). In our context, “epigenetics” refers to modifications to DNA or histones that aberrantly switch genes that promote or protect against cancer on or off, without changing the genetic sequence of DNA. No such epigenetic-based therapies currently exist for ocular cancers because epigenetic regulation of ocular cancers remains poorly understood. We’re working to help change that. Here’s our story so far...
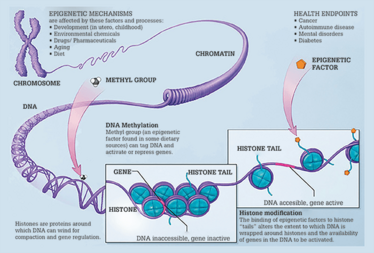
Epigenetics Explained
Image credit: The National Cancer Institute.
Expanding the horizon with epigenetics
When we first started paying attention to epigenetics in 2008, the focus was on histone methylation – the addition of methyl groups to histone tails and how that affects gene expression. Though a “hot” area, no one had really examined it in the developing mammalian retina. So we decided to investigate, and published a paper showing how the histone and methyl marks change during retinal development in the mouse (1). We discovered some interesting trends: a lot of these histone marks were upregulated in the inner retina, and some of the enzymes involved were developmentally regulated. One of these, the histone methyl-transferase EZH2, was expressed only during the growth phase of the retina, and then switched off when the retina was formed. Interestingly EZH2 was emerging as a major target for cancer therapies because it appears to be enriched in cells that grow quickly, such as fetal cells as well as cancer cells.
From studying the developing human retinae, we found that EZH2 was highly expressed in fetal retinae, but not postnatally (2). Because embryonic proteins can be expressed in cancer cells (3), we studied retinoblastoma samples, and found that EZH2 was highly expressed in the tumor cells from this childhood cancer. We also found it to be a good biomarker; immunohistochemistry on these tumor samples for EZH2 was almost a black and white indication of where tumor cells are… and where they are not. Histopathologic detection of EZH2 expression allowed identification of single tumor cells that were invading into the optic nerve or adjacent tissues. Because the decision to use systemic chemotherapy is linked to whether retinoblastoma cells have spread to the optic nerve – and beyond – staining these specific markers could help provide better indications of whether further treatment beyond surgery is actually warranted.
EZH2 was already under scrutiny by several companies, and small molecule inhibitors against it were in trials for other tumor types, such as lymphoma. We tested some of those inhibitors and found that they selectively killed the retinoblastoma cells, sparing the normal retinal cells. This was our entry point and, since then, we’ve published papers showing high levels of EZH2 in different tumors including vitreoretinal and orbital lymphomas, medulloepithelioma, and basal cell skin cancer, which can occur on the eyelid and the orbit, where it is difficult to treat (4)(5)(6). Right now, we are looking at some of the pathways downstream of EZH2, including DNA methylation.
A precise approach
An important part of our studies is to help patients with ocular cancers gain access to more targeted treatments. A close collaborator, Scott Tomlins, helped develop the panel for the National Cancer Institute (NCI) MATCH trial (See “The NCI MATCH Trial”). Together, we’ve been using the same technology to study eye and orbit tumors. But because ocular cancers are quite rare – there are only about five thousand cases per year in the United States (7) – acquiring tissue for study can be challenging. I use the analogy that studying cancer and human tissues is like studying freshwater; just like most freshwater is “locked up” in ice at the poles, most human tissues are embedded in wax and archived in hospitals and medical centers. But this fixation process and the wax can make downstream research applications more difficult, especially when trying to study the epigenetics. It’s why we’ve had to take a unique approach.
Using a scalpel, we “shave” off sections of samples to collect DNA, which we then put on a next-generation sequencing (NGS) panel (similar to NCI MATCH) to find mutations, gene alterations or copy number changes in those tumors. The panel is enriched for gene targets for which drugs have already been approved by the FDA (or in trial) for other cancer indications. So far, we’ve discovered many actionable alterations in genes, including MYD88, ARID1A, EZH2, PTEN, TP53, HRAS and NRAS (2)(4)(5)(6),(8). We’ve also found that eye lymphomas have a certain “flavor” and abundance of mutations that are not present elsewhere; MYD88 was commonly mutated in orbital marginal zone lymphomas, but uncommonly in marginal zone lymphomas elsewhere in the body (6). As there is already a drug in trial against the mutation we identified, we hope that our orbital lymphoma patients might be attractive candidates.

The NCI-MATCH Trial
The NCI-MATCH Trial (NCT02465060) is an ongoing precision medicine cancer treatment trial (11). In this study, biopsies from patients are analyzed using an NGS-based panel to identify actionable genomic alterations for precision medicine-based treatment strategies. Patients with advanced solid tumors, lymphomas, or myeloma who have progressed on standard treatment for their cancer, or patients with a rare cancer for which there is no standard treatment, are eligible for MATCH. Currently, there are 19 treatment arms open to patients, including genetic changes in EGFR, ALK and mTOR (11). In NCI-MATCH “basket trial,” patients can be enrolled in a trial no matter what kind of cancer they have, provided they have the same mutation that the trial drug is targeting. The trial utilizes the Oncomine Comprehensive Panel (OCP) to detect genomic variants in patient samples (12). The OCP was developed from analysis of over 700,000 tumor samples, and combination of genomic alterations with available therapeutics and ongoing clinical trials.
Image credit: The National Cancer Institute.
We’re basically looking for the “low hanging fruit” – tumors that haven’t yet been sequenced. And with orbit and eye tumors being so much rarer compared with other cancers, we have had to dig deep into our archives or collaborate with other centers to find tumor samples for study; in some cases we are analyzing samples that are 30 years old! But science and sequencing technologies have moved so fast that for relatively little money we can use small amounts (as little as 5 ng of tumor DNA) of these archived samples – including those that we thought were “locked up in ice” – and still retrieve usable information. Our initial goal is for patients with eye cancer to have the same options and treatments as patients who have other cancers through basket trials (clinical trials that target cancers based only on whether they contain specific genetic alterations, rather than the part of the body they come from). We hope to exploit drugs in our armamentarium that may be more specific than chemotherapy because they target genetic alterations present in the tumor but not in normal tissue. In the future, we want to help other ophthalmologists and ocular oncologists who see patients diagnosed with eye cancer by using these precision medicine strategies to identify diagnostic or druggable targets in their patients’ ocular cancers – and thus which clinical trials a patient may be eligible for. And if the drug receives approval, we’ll have made an important link in bridging a drug from other types of cancer or diseases to the field of eye cancer, and help our patients access more targeted therapies.
Why 'Sexy' Needs Substance
By Rajesh C. Rao
We all like to hear things in soundbites but, in my view, we should also explain what we mean when we use terms such as epigenetics, stem cells and precision medicine.
I’ve been in the stem cell field since 1999, and in epigenetics since 2008, and I think the term epigenetics is becoming like ‘stem cell’ in that it means many different things to different people. Scientists and clinicians have been expressing their concerns about how the term epigenetics can get misused in the media (13) – and we need to be more cautious with it. Why? Epigenetics could essentially mean anything; some of the influences are outside genetics. My concern is that using epigenetics as a ‘grab bag’ term is not helpful for science, patients or clinicians.
Whenever I talk about epigenetics, I quickly provide context of how I intend to use the term, stating that I am using it to refer to chemical modifications that occur to DNA and histones, and how these changes link to gene expression. Doing so brings me to a relatively focused area, so I can talk about some of the mechanisms driving the changes.
Going back to the stem cell analogy, some clinics state they are using stem cells – but don’t truly know if the “stem cells” they purport to use share defining characteristics of these cells such as self-renewal and tissue-specific differentiation (14). And in some cases, these clinics are putting patients in danger; take, for instance, the widely reported case of three female patients in Florida who suffered blindness as a result of an untested “stem cell therapy” (15).
Precision medicine is another grab-bag term. But haven’t we always been doing precision medicine? I am a retina specialist, and when I see a patient with macular degeneration or diabetic retinopathy, I routinely take into account their medical history such as whether they smoke and what medications they take, their A1C, and the findings from the retinal exam. One could (truthfully) say, “I’m practicing precision medicine!” – after all, the treatments are being tailored to the patient based on the unique characteristics of their disease. So again, rather than using ‘precision medicine’ as a grab bag term, I try to contextualize my usage: “By precision medicine, I mean that the patient has particular germline or somatic genetic changes (mutations or copy number alterations) or epigenetic changes (over expression or under expression of specific genes) – and based on those genetic or epigenetic alterations, I can now link the patient’s disease to a more tailored diagnosis, treatment, or experimental intervention being tested in a clinical trial.”
The bottom line? The moment we start using specialized terms, such as epigenetics, stem cells and precision medicine, we should also define them and include the context of how we are using them to describe our patients or their treatments.
A call for collaboration
We’re also hoping to improve diagnosis. Vitreoretinal lymphoma is rare – there are only around 400 cases per year in the US (9). Because of its link to CNS (brain) lymphoma, it’s a deadly disease, with only a quarter of patients surviving more than five years after diagnosis (10). It represents a crucial unmet need, not only because there is no standardized treatment – but also because it is very difficult to diagnose. In small volume vitreous samples taken from four patients with confirmed or suspected vitreoretinal lymphoma, we identified alterations in MYD88, CDKN2A and PTEN, showing that it is feasible to perform targeted NGS on intraocular liquid biopsies (as small as 500 µl or 5 ng of DNA) and identify the presence of tumor-causing mutations or copy number alterations (8) (Figure 1).
This approach could potentially enhance vitreoretinal lymphoma diagnosis and influence patient care. For instance, prior vitreous biopsies from one of the study cases had all been read as cytologically negative, with neither eye showing the presence of cancer cells. Two years after initial consultation, the patient presented with vision loss and right hemianopia; he had a brain lymphoma mass that was pressing on his visual centers. When we analyzed his original vitreous samples which had been stored in the freezer when collected two years prior to the brain lymphoma, we found tumor DNA confirming what later showed up in the brain: diffuse large B-cell lymphoma. Vitreoretinal lymphoma can be difficult to diagnose through standard cytology approaches, but because our test is so sensitive, as little as 5 or 6 ng of DNA is needed – which can come from just a few tumor cells in the eye. In the near future, we’d like to develop a diagnostic test that can be used by anybody. We already have the basis for the test, but because our research was only based on four samples – about one percent of all cases in the US – we want to collaborate with others; we need more samples to show that diagnosis using this precision medicine approach could be accurate and beneficial.
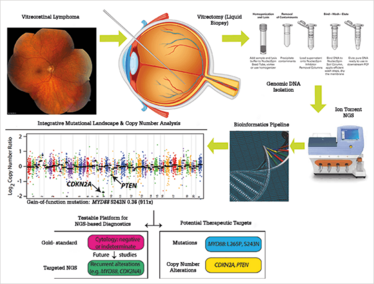
Figure 1. Workflow of determining driver and potentially actionable genomic alterations in vitreoretinal lymphoma. Adapted from (8).
Making strides forwards
The key take home message is this: the technology we need is there, but to make more progress in the field, different teams need to talk. Just as ophthalmology has led the way in stem cells and gene therapy, we can learn from other fields that are leading in precision medicine, and then apply it to ocular oncology. We can use today’s technologies to make powerful advances, to improve both diagnosis and treatment for our patients. Because ocular tumors are so rare, collaboration is really the key – it helps us bring the power of NGS, “big data” bioinformatics, precision medicine and epigenetic technologies to bear on this intractable problem.
Rajesh C. Rao is vitreoretinal surgeon, clinician-scientist, Assistant Professor of Ophthalmology and Visual Sciences at the Kellogg Eye Center, and Assistant Professor of Pathology, at the University of Michigan, USA. Rao is also the Leslie H. and Abigail S. Wexner Emerging Scholar at the A. Alfred Taubman Medical Research Institute, University of Michigan.
- RC Rao et al., “Dynamic patterns of histone lysine methylation in the developing retina”, Invest Ophthalmol Vis Sci, 51, 6784–6792 (2010). PMID: 20671280.
- M Khan et al., “Characterization and pharmacologic targeting of EZH2, a fetal retinal protein and epigenetic regulator, in human retinoblastoma”, Lab Invest, 95, 1278–1290 (2015). PMID: 26280220.
- M Monk and C Holding. “Human embryonic genes re-expressed in cancer cells”, Oncogene, 20, 8085–8091 (2001). PMID: 1178182.
- RC Rao et al., “EZH2, proliferation rate, and aggressive tumor subtypes in cutaneous basal cell carcinoma”, JAMA Oncol, 2, 962–963 (2016). PMID: 27054919.
- SE Avedschmidt et al., “The targetable epigenetic tumor protein EZH2 is enriched in intraocular medulloepithelioma”, Invest Ophthalmol Vis Sci, 57, 6242–6246 (2016). PMID: 27842164.
- AK Cani et al., “Comprehensive genomic profiling of orbital and ocular adnexal lymphomas identifies frequent alterations in MYD88 and chromatin modifiers: new routes to targeted therapies”, Mod Pathol, 29, 685–697 (2016). PMID: 27102345.
- Cancer.org, “What are the key statistics for eye cancer?” (2017). Available at: bit.ly/EyeStats. Accessed June 13, 2017.
- AK Cani et al., “Next generation sequencing of vitreoretinal lymphomas from small volume intraocular liquid biopsies: new routes to targeted therapies”, Oncotarget, 8, 7989–7998 (2017). PMID: 28002793.
- CC Chan et al., “Primary vitreoretinal lymphoma: a report from an International Primary Central Nervous System Lymphoma Collaborative Group Symposium”, Oncologist, 16, 1589–1599 (2011). PMID: 22045784.
- University of Michigan Research, “Out of sight”, (2016). Available at: bit.ly/UMichigan. Accessed June 13, 2017.
- National Cancer Institute, “NCI-MATCH Trial (Molecular Analysis for Therapy Choice)”, (2015). Available at: bit.ly/MatchTrial. Accessed June 13, 2017.
- DH Hovelson et al., “Development and validation of a scalable next-generation sequencing system for assessing relevant somatic variants in solid tumors”, Neoplasia, 17, 385–399 (2015). PMID: 25925381.
- Chris Woolston. “Researcher under fire for New Yorker epigenetics article”, Nature (2016). Available at: bit.ly/Woolston. Accessed July 19, 2017.
- RC Rao et al., “Stem cells for retinal disease: a perspective on the promise and perils”, Am J Ophthalmol, 179, 32–38 (2017). PMID: 28428049.
- E Kuriyan et al., “Vision loss after intravitreal injection of autologous ‘stem cells’ for AMD”, N Engl J Med, 376, 1047–1053 (2017). PMID: 28296617.
Rajesh Rao is vitreoretinal surgeon, clinician-scientist, Assistant Professor of Ophthalmology and Visual Sciences at the Kellogg Eye Center, and Assistant Professor of Pathology, at the University of Michigan, USA. Rao is also the Leslie H. and Abigail S. Wexner Emerging Scholar at the A. Alfred Taubman Medical Research Institute, University of Michigan.